Treatment of radiation injury in the adult
INTRODUCTION — The occurrence of industrial and medical radiation accidents and the threat of terrorist events involving radioactive material mandate the development and implementation of an appropriate medical response. Medical professionals who would logically be involved in such events include, among others, radiation safety officers, radiologists, radiation oncologists, nuclear medicine physicians, emergency department physicians, hematologists, medical oncologists, gastroenterologists, infectious disease specialists, as well as primary care providers. All will be asked to play a significant role in evaluating and treating victims of an accidental or deliberate exposure to radiation. Due to their experience in managing patients with cytopenias and/or marrow aplasia, hematologists will most likely be asked to take primary or consultative responsibility for medically treating individuals exposed to a moderate or high dose of radiation.
However, all physicians, and especially medical triage personnel, must have an understanding of how radiation alters the function of cells, tissues, and organ systems, how radiation levels are quantified, and how victims receiving a significant radiation dose can be recognized and categorized. These issues are discussed separately.
Scenarios have been developed for response to terrorist events resulting in small volume as well as mass casualties. The Strategic National Stockpile Radiation Working Group has developed a consensus opinion to provide guidance for estimating radiation dose, clinical assessment of exposed individuals, and medical management of those patients suffering from acute radiation injury [1]. Responding medical personnel must also be aware of local, state, and national resources that may be employed in the case of a radiation accident from whatever cause [2]. These subjects, as well as the treatment of patients with radiation injuries, will be discussed here.
Treatment of radiation accidents in children is covered separately.
SCENARIOS FOR RADIATION ACCIDENTS — Excessive radiation doses may result from a number of different exposures, as described below:
Accidental — Accidental exposure involves the release of radioactivity from small, usually sealed, sources (ie, nuclear medicine, brachytherapy, industrial gauges, small calibration sources), accidental overtreatment with radiation therapy, transportation accidents, and nuclear power plant accidents.
With the exception of accidents at nuclear reactor sites, such as Chernobyl, such exposures have usually involved only a small number of persons and a small area of nuclear contamination.
Deliberate — Examples of deliberate exposure to radiation might include [3]:
- An attack on a nuclear power plant
- A malevolent act using simple radiologic devices, such as sealed sources of radiation
- Terrorist use of a radiological dispersal device (RDD or "dirty bomb") using a small or large source of radioactivity and/or spent nuclear fuel
- Detonation of an improvised nuclear device (IND) or a nuclear weapon using a critical mass of fissionable material (eg, weapons-grade uranium or plutonium)
The two most likely scenarios would involve either an RDD or IND, with the former being more probable. Both warrant further discussion.
Radiologic dispersion devices — According to the United States Federal Government's accounting office, approximately 10 million "sealed sources" of radioactive material exist in 50 countries, including the United States [4]. These sources of radioactive material (eg, Cesium-137, Strontium-90, Cobalt-60, Plutonium-238, Plutonium-239) are encased in metal and are used in equipment for medical, industrial, agricultural, and research purposes. Of the 612 sealed sources that were reported lost or stolen since 1995, 254 have not been recovered. Many additional sealed sources may be unaccounted for as well.
Such material may be used by terrorists for making an RDD. When used with conventional explosives, radioactive substances may be dispersed over a relatively limited area (eg, a few city blocks) with the intent to cause fear or panic [3,5]. RDDs prepared with a radioactive powder, solution, or gas may be dispersed over a larger area, and pose a minimal radiation threat, but will result in a large number of persons presenting for concerns of radiation exposure.
An important exception to this is the scenario in which the patient is imbedded with radioactive fragments or shrapnel. These will be highly radioactive and can result in significant radionecrosis of local tissue in a short period of time, requiring urgent removal. Procedures for removing such fragments are described below.
Improvised nuclear devices — An improvised nuclear device (IND) employs radioactive material which, following detonation, results in a nuclear reaction (eg, atom bomb, hydrogen bomb). Fission, the splitting of the atom, is exploited in a nuclear detonation. An uncontrolled fission chain reaction generates an enormous amount of energy in a small period of time. This process results in the generation of three forms of energy, which are released from such nuclear explosions:
- Heat (approximately 35 percent of total energy)
- Shock or bomb blast (approximately 50 percent)
- Radiation (approximately 15 percent)
The blast wave from a nuclear explosion results in fractures, lacerations, rupture of viscera, pulmonary edema, hemorrhage, and embolic events, while the thermal energy causes flash burns, flame burns, flash blindness, and retinal burns. Regardless of the source of radioactive material, the presence of multiple injuries is a mortality multiplier, owing to the predisposition to infection from trauma and burns, compounded by the immunosuppression and cytopenias caused by radiation doses as low as 0.5 Gy.
As an example, it has been estimated that 65 to 70 percent of the injuries sustained in a nuclear war will be varying combinations of burns, wounds, and irradiation, while the remainder will be single injuries equally divided between irradiation and burns.
Generation of radionuclides — The generation of radionuclides consequent to a nuclear weapon detonation occurs as a result of byproduct generation during nuclear fission as well as through neutron activation of stable elements, which are usually ground sources (eg, soil). The primary fission products, radionuclides, constitute a spectrum of hundreds of species with differing half-lives and varying biologic importance.
Many of these nuclides are the starting point of their own decay chain. These radionuclides continue to decay, releasing radiation, until they finally become stable. The principal nuclides per megaton of fission are shown in the table (table 1). Knowledge of these radionuclides becomes important and clinically meaningful as may be encountered during or subsequent to fallout. The clinician may encounter them in an externally or internally contaminated patient.
Yields of radionuclides from nuclear fission
|
Radionuclide |
Half-life |
Yield (MCi per megaton) |
|
Iodine-131 |
8 days |
125 |
|
Cerium-131 |
1 year |
39 |
|
Zirconium-95 |
65 days |
25 |
|
Strontium-89 |
53 days |
20 |
|
Ruthenium-103 |
40 days |
18 |
|
Cerium-144 |
33 days |
4 |
|
Ruthenium-106 |
1 year |
0.3 |
|
Cesium-137 |
30 years |
0.2 |
|
Strontium-90 |
28 years |
0.1 |
This table shows some of the most important radionuclides produced during explosion of a nuclear fission device. Yields are expressed as millicuries (MCi) per megaton.
From The Medical NBC Battlebook United States Army CHPPM, Technical Guide 244, August, 2002.
INITIAL TRIAGE — In the case of an accident or intentional event involving nuclear material, the first responders will likely include members of a HAZMAT team, local fire and police departments, and individuals knowledgeable in radiological monitoring from a state agency, such as the State Department of Environmental Protection. Many states have or will be setting up Weapons of Mass Destruction- Civil Support Teams, which can significantly augment the command system and can deploy within four hours at the request of a governor or the President of the United States.
With the advent of the Department of Homeland Security (DHS), numerous monetary grants have been awarded to enhance the capabilities of first responders. Moreover, DHS's significant restructuring of numerous federal agencies has unified numerous efforts. One of the seminal efforts has been the development of the National Response Plan (NRP). The NRP is a single all-discipline, all-hazards plan. This comprehensive plan revolutionizes the federal response to terrorism, major disasters, and other emergencies by treating crisis management and consequent management as a single integrated function under DHS.
The NRP also includes the implementation of the National Incident Management System (NIMS) to ensure that all levels of government are able to work together during a disaster. In the event of a significant detonation, the Initial NRP calls for self deployment of several federal assets and agencies, including the Federal Bureau of Investigation [6,7]. Their responsibilities are to manage the consequences of the incident by means of the following [1,3,5]:
- Protecting the public
- Limiting further damage
- Monitoring the extent and types of radioactivity present
- Performing decontamination
- Disposing of radioactive material
- Making decisions concerning evacuation, relocation, shelter, need for potassium iodide, as well as guidance for other protective actions
Medical centers, in turn, must develop and rehearse radiation response plans that coordinate their efforts with those of local, state, regional, and national response teams.
Prehospital triage — Initial triage will be performed by first-responders, who will not enter a radiation environment until the extent of the hazard is known. A HAZMAT team will likely self-deploy and arrive on the scene early on to guide other responders. Some first responders may carry electronic pocket dosimeters that would alert them to the presence of radiation. All participants should be volunteers whenever possible.
First responders should work in teams and should be monitored with physical dosimetry if possible. In a true emergency, the equivalent dose to a large portion of an emergency responder's body may approach 0.5 Sv (50 rem) in a short time. The volunteer needs to understand the associated risk for potential acute effects, which are minimal to none, but that there may be some increased risk for subsequent malignancy.
First responders will receive protective action guidance. Early on, data may be sparse, and this will be based on the best scientific guess. Protective gear should include eye protection, respiratory protection, gloves, and physical dosimetry if possible. Clothes and a fire fighter's bunker gear will afford some protection of the skin. First responders and all other health care providers must use strict isolation precautions (disposable gowns, double gloves, masks, cap, shoe covers) for personal protection [3,8]. Outer gloves should be changed often to avoid cross-contamination. Protective gear should be removed after use and placed in a clearly labeled, sealed plastic container.
Early management in the field and the emergency department should follow basic triage principles (table 2):
- Life-threatening injuries, if present, should be treated even before assessing the amount of radiation exposure. It should be assumed that all victims are contaminated, either by absorption of radiation through the skin after being physically covered by radioactive material or by ingestion or by inhalation of radioactive material. Victims should be stabilized and transported to a medical facility.
- Injured victims should be treated by standard triage guidelines. Preliminary decontamination (ie, removal of clothing, washing of the victim) should remove 90 to 95 percent of external contamination.
- If there are many victims, persons who are externally contaminated and are without other injury should be relocated to an upwind site other than the hospital in order to decongest the hospital care system. Thereafter, assessment and prevention of contamination, treatment of minor injuries, and evaluation and treatment of internal contamination should be addressed [3].
Triage considerations: nuclear detonation
|
Conventional triage for injuries with no radiation exposure* |
Triage Categories for those with injuries (eg, burns, trauma) in addition to radiation exposure |
||
|
<1.5 Gy |
1.5-4.5 Gy |
4.5-10 Gy |
|
|
Delayed |
Delayed |
Variable |
Expectant |
|
Immediate |
Immediate |
Immediate |
Expectant |
|
Minimal |
Minimal |
Minimal |
Minimal |
|
Expectant |
Expectant |
Expectant |
Expectant |
|
Absent |
Ambulatory• |
As needed• |
As needed• |
*
This column contains the conventional military triage treatment system for
subjects with significant mechanical trauma or burns. The categories are defined
as follows: Delayed treatment: Medically stable with significant injury, but
may survive until definitive treatment is available; Immediate treatment:
Subjects with high survivability and significant injury, provided that
immediate therapy is available; Minimal therapy: Medically stable subjects with
minor injury; Expectant therapy: Subjects who are seriously injured in whom
survivability is poor.
• Subjects with radiation injury alone and an exposure of <1.5 Gy should be
monitored in an ambulatory setting. Those with exposures >1.5 Gy should be
given routine care (eg, cytokines, antimicrobial agents, transfusions,
laboratory monitoring) and hospitalization, if required, as indicated in the
text.
Waselenko, JK, et al. Ann Intern Med 2004; 140:1037.
Removal of radioactive fragments — Providers involved in the removal of radioactive fragments or shrapnel from an exploded device must first consult the radiation safety officer (RSO). Shielding barriers, which are found in many operating rooms owing to their need in brachytherapy insertion and removal, will afford some protection.
Finger ring dosimeters should be worn by physicians removing such fragments. At a minimum they should be worn on the dominant hand, although having one on each hand is optimal. Unfortunately, these dosimeters are not read locally. However, an electronic pocket dosimeter (EPD) could be taped on the forearm, under the gown, for real-time reading. The RSO can then calculate the dose to the fingers based on this reading and the operating distance.
Physicians should work in teams with frequent monitoring of radiation doses so that exposure time can be minimized; pregnant personnel should be excluded from such efforts. Removed fragments should be placed into a lead container and covered. Both finger ring dosimeters and suitable lead containers are available from the medical center's Nuclear Medicine department. These steps should significantly minimize the risk to the provider and lessen their risk of local radiation injury.
In hospital triage — Health care providers should be well-trained and rehearsed and must also use strict isolation precautions (eg, disposable gowns, double gloves, masks, cap, eye protection, and shoe covers) for personal protection [3,8]. Inner gloves should be taped to the gown and outer gloves should be changed often to avoid cross-contamination. If possible, contaminated patients should enter the treatment facility through a separate entrance.
Ideally, physical dosimeters should be worn under the gown and monitored to ensure provider safety, but this should not preclude caring for the patient. Protective gear should be removed after use and placed in a clearly labeled, sealed plastic container. Hospital personnel should also be monitored for contamination prior to leaving the area or after decontaminating themselves.
Safety of health care providers — The safety of health care providers is of paramount importance. Health care providers should approach the patient as though he or she has been contaminated with human blood, body fluids, or raw sewage. This requires donning a gown, mask, double gloves, cap, and shoe covers. Outer gloves should be changed frequently to avoid cross-contamination. Following use, protective gear should be removed and placed in a labeled, sealed plastic container.
Provided that these universal precautions are taken, it is extremely unlikely that radioactive contamination will occur, even when treating a patient with a heavy burden of radioactive material. In fact, there are no reports of health care workers who have adhered to this protocol becoming contaminated from handling such patients [1]. All hospital personnel should be assessed for contamination when leaving the treatment area and decontaminated, if required.
Additional precautions need to be taken when the patient is imbedded with radioactive fragments. These are discussed above.
CLINICAL ASSESSMENT — After arrival in the emergency department, victims should be classified based on whether or not they have been contaminated with radioactive material, received a significant external radiation exposure without contamination, and/or received physical injury.
The vast majority of individuals arriving in the emergency department after an event involving an RDD are likely to have insignificant or no exposure. Clinicians should be able to identify those victims whose exposure is significant, using principles presented separately.
When necessary, and if not already performed, victims should be decontaminated after clinical assessment of injury severity has been made. Depending on the situation, a trauma surgeon, burn specialist, dermatologist, gastroenterologist, and/or neurologist may be consulted, in addition to the hematologist. Information regarding risk level should be provided to medical caregivers by the medical center's radiation safety officer, radiologist, nuclear medicine physician, and/or radiation oncologist.
History taking — Historical information, including the location of the incident, duration of exposure, interval between exposure and clinical evaluation, activity and exact location at the time of exposure, and occupation of the victim should be documented in the medical record. Other information, such as a general description of the accident, source of radiation, and numbers of individuals involved in the exposure should be documented, whenever possible.
Generally, the clinical signs and symptoms of radiation exposure are nonspecific. However, the presence or absence of nausea, vomiting, diarrhea, abdominal cramping and/or bleeding, fatigue, fever, and mental changes should be noted. If the patient has experienced vomiting, the time of onset after the exposure should be noted as accurately as possible, since such information is of extreme importance in estimating the degree of radiation exposure (table 3).
Radiation biodosimetry
|
Dose (Gy) |
Vomiting (%) |
Time to vomiting (hours) |
ALC day 1 (/microL) |
Lymphocyte fall rate constant (k)* |
Lymphocyte dicentrics (per 1000) |
|
0 |
0 |
- |
2450 |
- |
1-2 |
|
1 |
19 |
- |
2160 |
0.126 |
88 |
|
2 |
35 |
4.6 |
1900 |
0.252 |
234 |
|
3 |
54 |
2.6 |
1680 |
0.378 |
439 |
|
4 |
72 |
1.7 |
1480 |
0.504 |
703 |
|
5 |
86 |
1.3 |
1310 |
0.63 |
1000 |
|
6 |
94 |
1.0 |
1150 |
0.756 |
|
|
7 |
98 |
0.8 |
1010 |
0.881 |
|
|
8 |
99 |
0.7 |
890 |
1.01 |
|
|
9 |
100 |
0.6 |
790 |
1.13 |
|
|
10 |
100 |
0.5 |
700 |
1.26 |
|
Gy:
absorbed whole body dose in Grey units; ALC: absolute lymphocyte count per
microL.
* The lymphocyte fall rate constant is derived from a semilogarithmic plot of
the absolute lymphocyte count (ALC) versus time in days, in the form of 2450 x
e(-kt). The time (in days) for the ALC to fall to one-half of its original
value [half-time, T(1/2)] can be obtained from the following equation: T(1/2) =
0.693/k.
Modified with permission from: Waselenko, JK, MacVittie, TJ, Blakely, WF, et al. Medical management of the acute radiation syndrome: Recommendations of the strategic national stockpile radiation working group. Ann Int Med 2004; 140:1039. Copyright © 2004 American College of Physicians.
Physical examination — The physical examination should include vital signs (fever, hypotension, orthostatic changes), skin examination (erythema, blistering, edema, desquamation), neurologic examination (level of consciousness, ataxia, motor/sensory deficits, presence or absence of reflexes, papilledema), gastrointestinal examination (abdominal tenderness, gastrointestinal bleeding) and hematologic examination (ecchymoses and/or petechiae of mucous membranes and skin).
A schema has been developed to assess the severity of changes in the clinical examination according to standardized cutaneous (table 4), gastrointestinal (table 5), cerebrovascular (table 6), and hematopoietic (table 7) radiation injury scoring systems.
Radiation toxicity: cutaneous system
|
Symptom/sign |
Degree1 |
Degree 2 |
Degree 3 |
Degree 4 |
|
Erythema |
Minimal, transient |
Moderate <10 percent BSA |
Marked 10-40 percent BSA |
Severe >40 percent BSA |
|
Sensation/itching |
Pruritus |
Slight, int. pain |
Moderate persistent pain |
Severe persistent pain |
|
Blistering |
Rare |
Rare hemorrhage |
Bullae |
Bullae hemorrhage |
|
Desquamation |
Absent |
Patchy, dry |
Patchy, moist |
Confluent, moist |
|
Ulcer/necrosis |
Epidermal only |
Dermal |
Subcutaneous |
Muscle or bone |
|
Onycholysis |
Absent |
Partial |
Partial |
Complete |
BSA: body surface area; Int: intermittent.
Modified with permission from: Waselenko, JK, MacVittie, TJ, Blakely, WF, et al. Medical management of the acute radiation syndrome: Recommendations of the strategic national stockpile radiation working group. Ann Int Med 2004; 140:1039. Copyright ©2004 American College of Physicians.
Radiation toxicity: gastrointestinal system
|
Symptom |
Degree 1 |
Degree 2 |
Degree 3 |
Degree 4 |
|
Stool (#/day) |
2-3 |
4-6 |
7-9 |
≥10 |
|
Stool consistency |
Bulky |
Loose |
Loose |
Watery |
|
GI bleeding |
Occult |
Intermittent |
Persistent |
Persistent large amount |
|
Abdominal cramps or pain |
Minimal |
Moderate |
Intense |
Excruciating |
Modified with permission from: Waselenko, JK, MacVittie, TJ, Blakely, WF, et al. Medical management of the acute radiation syndrome: Recommendations of the strategic national stockpile radiation working group. Ann Int Med 2004; 140:1039. Copyright © 2004 American College of Physicians.
Radiation toxicity: cerebrovascular system
|
Symptom |
Degree 1 |
Degree 2 |
Degree 3 |
Degree 4 |
|
Nausea |
Mild |
Moderate |
Intense |
Excruciating |
|
Vomiting |
once/day |
2-5 times/day |
6-10/day |
>10/day |
|
Anorexia |
Able to eat |
Decreased intake |
Minimal intake |
Parenteral nutrition needed |
|
Fatigue |
Able to work |
Work impaired |
Assistance for ADL |
Cannot do ADL |
|
Temp (ºC) |
<38 |
38-40 |
>40 for <24 hrs. |
>40 for >24 hrs. |
|
Headache |
Minimal |
Moderate |
Intense |
Excruciating |
|
BP (mmHg) |
>100/70 |
<100/70 |
<90/60 |
<80 systolic |
|
Neurologic deficits* |
Barely detected |
Easily detected |
Prominent |
Life-threatening LOC |
|
Cognitive deficits• |
Minor loss |
Moderate loss |
Major impairment |
Complete impairment |
ADL:
activities of daily living; Temp: temperature; BP: blood pressure; LOC: loss of
consciousness.
* Reflexes (including corneal), papilledema, seizures, ataxia, other motor and
sensory signs.
• Impaired memory, reasoning, or judgement.
Modified with permission from: Waselenko, JK, MacVittie, TJ, Blakely, WF, et al. Medical management of the acute radiation syndrome: Recommendations of the strategic national stockpile radiation working group. Ann Int Med 2004; 140:1039. Copyright © 2004 American College of Physicians.
Levels of hematopoietic toxicity following radiation exposure
|
Degree |
ALC |
ANC |
Platelet count |
Bleeding and anemia |
|
0* |
1400-3500 |
4000-9000 |
140-400,000 |
None |
|
1 |
≥1500 |
≥2000 |
≥100,000 |
Petechie, bruising |
|
Normal Hgb level |
||||
|
2 |
1000-1500 |
1000-2000 |
50-100,000 |
Mild blood loss |
|
<10 percent decrease in Hgb |
||||
|
3 |
500-1000 |
500-1000 |
20-50,000 |
Gross blood loss |
|
10-20 percent decrease in Hgb |
||||
|
4 |
<500 |
<500 |
<20,000 |
Spontaneous bleeding |
|
>20 percent decrease in Hgb |
ALC:
absolute lymphocyte count in cells/microL; ANC: absolute neutrophil count in
cells/microL; Platelet count in cells/microL; Hgb: hemoglobin concentration.
* Degree 0 represents normal reference values.
Modified with permission from: Waselenko, JK, MacVittie, TJ, Blakely, WF, et al. Medical management of the acute radiation syndrome: Recommendations of the strategic national stockpile radiation working group. Ann Int Med 2004; 140:1039. Copyright ©2004 American College of Physicians.
Initial laboratory testing — If internal contamination is suspected, collection and monitoring of secretions and excreta can be helpful. For example, obtaining bilateral nasal swab samples within the first hour of the incident can provide valuable information. As an example, the extent of nares contamination is approximately 5 percent of that received by the pulmonary alveoli. For victims in whom internal contamination is suspected, peripheral blood (for the same tests as ordered for an external exposure), urine, nasal smears, spontaneous vomitus, and stools should be obtained for radiological monitoring. Hospital staff must take precautions with the handling of these samples as they may be radioactive. Any patient with wound contamination or imbedded with radioactive fragments should be evaluated for such internal contamination.
Initial laboratory testing should include a complete blood count (CBC) with white blood cell differential and platelet count, along with routine chemistry tests. The time of CBC collection must be carefully noted, because of important time-related changes in the lymphocyte count (table 3).
If possible, serial CBCs should then be obtained every 6 to 12 hours for at least three samples. Twenty-four hours after any significant exposure, a blood sample should be drawn into a lithium heparin tube and sent to an appropriate referral lab for confirmatory chromosomal aberration analysis. This information may also aid in the patient's management and the determination of overall prognosis (table 3).
Additional monitoring should be based on the whole-body dose, as the onset of neutropenia and its severity are dose dependent (figure 1). Patients with low exposures may need a weekly or twice-weekly CBC for 4 to 6 weeks to document their WBC nadir and subsequent recovery.
For patients felt to have internal contamination, a 24-hour urine and stool sample every day for four days should be collected and analyzed for radionuclide contamination. Treatment guidance should be based on expert assistance, such as that obtained from the NCRP Report 65, Management of Persons Accidentally Contaminated with Radionuclides. Advice is also available on the following website:www.orau.gov/reacts.
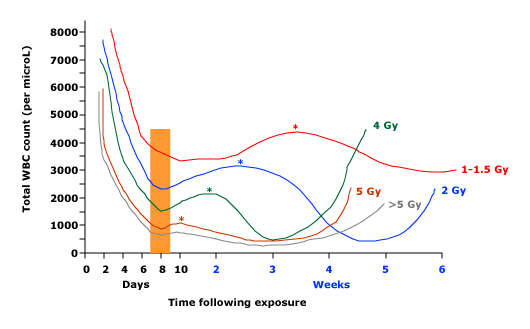
This graph shows serial changes in the total white blood cell count (WBC, vertical axis) as a function of the time following radiation exposure (days, weeks; horizontal axis) for victims of the Chernobyl reactor accident. The data are separated into five groups, with exposures ranging from 1.0 to >5 Gy. Because of the profound radiation-induced lymphocytopenia at these doses, the total WBC counts shown here are almost entirely composed of neutrophils. Note that the time of the initial WBC nadir at 7 to 9 days post-exposure (shown in orange) is similar in all five exposure groups. This is followed by a transient ("abortive") rise, shown by the (*) symbol, in those groups receiving a dose of 5 Gy (500 rads) or less. A period of profound leukopenia/neutropenia follows this abortive rise, which may be delayed for up to 5 weeks in those with lower exposures (eg, 2 Gy). At the higher exposures (eg, ≥5 Gy), profound neutropenia may last for several weeks before recovery ensues.
Reproduced with permission from: Vorobiev, AI. Acute radiation disease and biological dosimetry in 1993. Stem Cells 1997; 15:269. Copyright © 1997 AlphaMed Press.
High risk populations
Pregnancy — The dose to the gravid uterus is approximately 65 to 70 percent of that received on the surface, affording some protection to the fetus from external radiation. However, when internal radiation contamination is present, the fetus may receive a high dose due to its proximity to the maternal bladder. In addition, the fetal thyroid begins to take up iodine after 12 weeks, adding to the potential for injury.
Because the fetus is very susceptible to the effects of ionizing radiation, any pregnant female exposed to radiation should also see a health physicist and a maternal fetal medicine specialist.
Children — Several unique features encountered in children enhance their vulnerability to the effects of radiation. This subject is discussed in detail separately.
Elderly — Increased susceptibility to radiation is also encountered in elderly patients. This results from an inherently diminished bone marrow reserve as well as the increased likelihood of co-morbidities, increasing the risk for development of anemia, bleeding, and/or infection.
INITIAL MANAGEMENT DECISIONS — Management decisions must be made for high-risk individuals when results of individual biodosimetry (eg, chromosomal analysis, lymphocyte kinetics) are not yet available. One approach to the decision-making process, developed by the Medical Treatment Protocols (METREPOL) team, is to assign a score based upon clinical and routine laboratory findings [9]. This application is very detailed and may be useful in a radiation accident in which a small number of casualties are present, but is impractical in a mass casualty scenario.
Integration of clinical information regarding the severity of signs and symptoms (table 4 and table 5 and table 6 and table 7), along with the presence and timing of the onset of vomiting, and changes in peripheral blood counts (table 3) permits one to assess the severity of exposure to ionizing radiation in quantitative terms.
A "response category" is assigned to each victim, determined by the highest degree of severity in any of the signs or symptoms [9]. Using this information and results of hematologic monitoring, victims can be triaged to the ambulatory setting, routine care medical/surgical floor, intensive care unit or transplantation unit, as outlined in the figure (figure 2) [10].
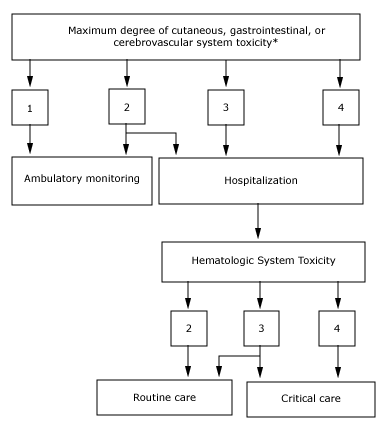
This flow chart details the triage and therapy for persons exposed to radiation in a scenario in which there are a limited number of casualties. The degree of toxicity to the variously defined organ systems (ie, cutaneous, gastrointestinal cerebrovascular, and hematologic, see separate figures) determines whether the patient is admitted to the hospital or monitored in an ambulatory setting. Patients with hematologic toxicity of grades 2 to 4 may be treated with transfusion of blood components, those with grades 3 to 4 may receive colony-stimulating factors, and those with grade 4 hematologic toxicity are potential candiates for hematopoietic cell transplantation.
* The highest degree of toxicity to any of these three organ system indicates
the physiologic "response category" for an individual patient. All
patients with hematologic toxicity of grade 2 or more require hospitalization.
Reproduced with permission from: Dainiak, N. Hematologic consequences of exposure to ionizing radiation. Exp Hematol 2002; 30:513. Copyright © 2004 Elsevier Inc
Assessing prognosis — Dose estimates provide an added level of certainty with regard to prognosis, and impact on selection of therapy (table 8 and table 9). In order to facilitate the integration of clinical, laboratory, and dosimetric data, a radiation casualty management software program (ie, the Biological Assessment Tool) has been developed by the Armed Forces Radiobiology Research Institute [11]. Background information and advice on clinical management of radiation incidents can be obtained at this website and at the website for REAC/TS (www.orau.gov/reacts).
Phases of radiation injury
|
Dose (Gy) |
Symptoms |
Prognosis |
|||
|
Prodrome |
Hematologic |
GI |
Neurologic |
||
|
0.5 to 1.0 |
+ |
+ |
0 |
0 |
Survival almost certain |
|
1.0 to 2.0 |
+/++ |
+ |
0 |
0 |
Survival >90 percent |
|
2.0 to 3.5 |
++ |
++ |
0 |
0 |
Probable survival |
|
3.5 to 5.5 |
+++ |
+++ |
+ |
0 |
Death in 50% at 3.5 to 6 wks |
|
5.5 to 7.5 |
+++ |
+++ |
++ |
0 |
Death probable in 2-3 wks |
|
7.5 to 10 |
+++ |
+++ |
+++ |
0* |
Death probable in 1-2.5 wks |
|
10 to 20 |
+++ |
+++ |
+++ |
+++ |
Death certain in 5-12 days |
|
>20 |
+++ |
+++ |
+++ |
+++• |
Death certain in 2-5 days |
Gy:
dose in Grey; GI: gastrointestinal side effects; 0: no effects; +: mild; ++:
moderate; +++: severe or marked.
* Hypotension.
• Also cardiovascular collapse, fever, shock.
Modified from: Waselenko, JK, MacVittie, TJ, Blakely, WF, et al. Medical management of the acute radiation syndrome: Recommendations of the strategic national stockpile radiation working group. Ann Int Med 2004; 140:1039.
Treatment guidelines for radiation exposure
|
Variable |
Cytokines |
Antibiotics |
HCT |
|
Less than 100 casualties |
|||
|
Healthy, no other injuries |
3 to 10* |
2 to 10 |
Allo: 7 to 10 |
|
Auto: 4 to 10 |
|||
|
Multiple injuries or burns |
2 to 6 |
2 to 6 |
NA |
|
More than 100 casualties |
|||
|
Healthy, no other injuries |
3 to 7 |
2 to 7 |
Allo: 7 to 10 |
|
Auto: 4 to 10 |
|||
|
Multiple injuries or burns |
2 to 6 |
2 to 6 |
NA |
HCT:
hematopoietic cell transplantation; Allo: allogeneic HCT; Auto: autologous HCT;
NA: not applicable; G-CSF: granulocyte colony-stimulating factor; GM-CSF:
granulocyte-macroplage colony-stimulating factor.
* This table provides a consensus guideline for treatment with cytokines (eg,
G-CSF, GM-CSF), antibiotics, and consideration for hematopoietic cell
transplantation based upon whole body or significant partial body exposure
doses, given in Gy units. See text for treatment details.
Modified with permission from: Waselenko, JK, MacVittie, TJ, Blakely, WF, et al. Medical management of the acute radiation syndrome: Recommendations of the strategic national stockpile radiation working group. Ann Int Med 2004; 140:1039. Copyright © 2004 American College of Physicians.
It is important to recognize those patients who may need no or minimal care, as well as those whose degree of radiation exposure precludes survival (table 2). These two groups are discussed below.
Minimally exposed patients — Patients with exposures of less than 0.5 to 1.0 Gy will invariably survive, provided there are no other life-threatening complications of the exposure (eg, bomb blast, burns, fractures). These patients can be recognized by the following signs and symptoms:
- No or minimal prodromal symptoms (ie, anorexia, apathy, nausea, vomiting, and/or diarrhea) (table 3 and table 8).
- No or minimal (degree 1) gastrointestinal system changes (table 5)
- No cerebrovascular system changes (table 6)
- No or minimal decline in lymphocyte count, absolute neutrophil count, or platelet count 24 to 48 hours after exposure (table 3 and table 7)
These patients do not require hospitalization, and may need no medical care. Nausea and vomiting, if present, are usually mild and transient, and usually abate within two to three days. Reassurance and psychological care are essential, however, especially in mass casualty settings. Accordingly, ambulatory monitoring with psychosocial support may be required.
Fatal outcome — Patients with exposures in excess of 10 to 12 Gy have virtually no chance of survival. Depending on therapy, death is certain within days to weeks following exposure, despite any and all treatments. Such patients will present with the following signs and symptoms:
- Onset of vomiting within 30 minutes to one hour following exposure (table 3).
- Severe or marked cerebrovascular system changes (degree 3 or 4) (table 6)
- Severe degrees of lymphopenia and/or marked decline in absolute lymphocyte count within 24 hours of exposure (table 3)
In a mass casualty scenario, a more simplified strategy employing military triage principles should be considered (table 2). This triage model focuses life saving efforts and resource expenditures on those with more survivable injuries and triages those with highly mortal wounds to the expectant category. Such patients should be provided with comfort measures, such as management of pain, vomiting, and diarrhea. Psychological support and pastoral care are essential for helping the patient and family through such devastating exposures
Psychosocial impact — The psychosocial impact of an act of terrorism cannot be overemphasized. Many victims will have psychological symptoms, ranging from insomnia and hypervigilance to social withdrawal [12]. Posttraumatic stress disorder may occur among victims, families, and friends. High-risk victims include children, pregnant women, mothers of young children, and victims with a prior medical history of psychiatric disorders. The principle of therapy is to establish trust through open communication. Approaches to management of behavioral and mental health problems in similar settings have been presented [13].
INITIAL MEDICAL AND SURGICAL MANAGEMENT
Surgery — Surgical intervention, when required, should be carried out within 36 hours, and not later than 48 hours after exposure [14]. Additional surgery, if required, should not be performed until at least six weeks post-exposure, in order to assure recovery from the period of cytopenia and immunosuppression, which would otherwise seriously add to the risk of developing surgical complications (ie, infection, poor wound healing). Precautions for removal of radioactive fragments are described above.
Nausea and vomiting — Given the importance of the time elapsed between radiation exposure and the onset of vomiting in determining individual radiation dose, prophylaxis against vomiting is not initially desired, and may also be impractical given the short time to onset of vomiting with clinically significant exposures (table 3) [15]. In addition, at low exposure doses, vomiting usually abates after 48 to 72 hours; therefore, prolonged antiemetic therapy is not usually warranted.
If treatment is required, the use of serotonin receptor antagonists is preferred [16]. Neuroleptic antiemetics may also be employed.
General supportive measures — Issues requiring active or preventative treatment include any or all of the following:
- Maintaining normal vital signs and assuring an open airway. These are especially important in those sustaining additional injuries (eg, blast damage, burns, trauma)
- Rapid replacement of fluid, electrolyte, and blood losses, especially in those presenting with shock, hypotension, significant burns, hypovolemia, and/or multiorgan failure shortly after exposure
- Seizure control, if present
- Control of nausea, vomiting, and/or diarrhea
- Judicious use of analgesics, anxiolytics, sedatives
Hematologic support (eg, transfusion of blood components, use of cytokines, hematopoietic cell transplantation) should be considered in those having estimated exposures in the range of 2 to 10 Gy. This subject is discussed in detail below.
Antibiotics — In non-neutropenic patients, use of antibiotics should be reserved for obvious foci of infection secondary to extensive burns, penetrating wounds, and/or abdominal/visceral trauma. Since altering the anaerobic gut flora has worsened outcomes in irradiated animals, antibacterial gut prophylaxis should only be administered in patients with an abdominal wound or C. difficile enterocolitis [17].
Thyroid protection — In the case of significant exposure to radioactive isotopes of iodine (eg, nuclear reactor incident, atomic blast), prevention of significant uptake of radioactive isotopes of Iodine, especially Iodine-131, by the thyroid is imperative. This is especially important in the exposed fetus after the 12th week of gestation, as well as in the child or adolescent, all of whom are most prone to the development of radiation-induced thyroid carcinoma. This form of the thyroid cancer also appears to be biologically more aggressive than de novo forms.
Potassium iodide (KI) is available in 130 mg tablets. A one-time oral dose of 130 mg is recommended for pregnant or lactating women and adults >18 years of age (table 10) [18]. Oral KI should be administered as soon as possible, preferably less than 6 hours after the exposure [19]. However, if it anticipated that a person will be exposed to radioactive iodine for more than 24 hours, additional doses should be taken every 24 hours. Guidance and KI recommendations will be provided by emergency management officials after an incident. Information on the use of potassium iodide as a thyroid blocking agent in radiation emergencies can be found on the FDA website at: <www.fda.gov/downloads/Drugs/GuidanceComplianceRegulatoryInformation/Guidances/ucm080542.pdf> [20].
Recommended doses of potassium iodide after radiation exposure
|
Age of patient |
Predicted thyroid dose (cGy) |
Daily dose of KI (mg)* |
|
>40 years |
≥ 500 |
130 |
|
>18 through 40 |
≥ 10 |
130 |
|
Pregnant or lactating |
≥ 5 |
130 |
|
>12 though 18 years |
≥ 5 |
65 |
|
>3 through 12 years |
≥ 5 |
65 |
|
>1 month through 3 years |
≥ 5 |
32 |
|
Birth through 1 month |
≥ 5 |
16 |
KI:
potassium iodide.
* Potassium iodide is available as 130 or 65 mg tablets, or as Lugol's
solution. KI must be used within 4 to 6 hours of exposure to block uptake of
radioactive iodine by the thyroid. If radioactive iodines are not part of the
radiation exposure, KI is not needed. See text for details.
Based on FDA Guidance, 2001. Available at <www.fda.gov/cder/guidance/4825fnl.htm>.
MANAGEMENT OF THE HEMATOPOIETIC RADIATION INJURY SYNDROME — Successful administration of supportive care in the
non-hematopoietic stem cell transplant scenario is dependent upon all of the following conditions being present:
- The nonhematopoietic injuries (eg, cerebrovascular, gastrointestinal, and cutaneous syndromes, as well as radiation-induced lung injury and other trauma) are survivable.
- Radiation-induced damage to hematopoietic stem and progenitor cells is reversible.
- Hematopoietic regeneration results in the production of adequate numbers of functionally normal neutrophils and platelets within the critical, clinically manageable period (ie, approximately two to six weeks following radiation exposure), or the patient will not survive.
Appropriate management of the hematologic complications of radiation injury requires judicious and prompt use of blood products, antibiotics, hematopoietic cytokines, as well as the possible use of hematopoietic cell transplantation in a select number of victims who have no other injuries or significant toxicity to other organs.
Physicians with experience in the clinical management of patients with prolonged cytopenias, complications of total body irradiation, and their infectious sequelae are an absolute requirement for management of patients with the hematopoietic radiation injury syndrome. This will likely involve hematologists, oncologists, and physicians skilled in hematopoietic cell transplantation. These patients will have additional complexity, owing to severe injuries to the cutaneous and mucosal barriers, as well as other radiation- or trauma-related organ toxicities. Specialists from all disciplines will be required in their management. These issues are discussed below [1,21].
Background — Early experimental work demonstrated the efficacy of supportive care following radiation exposures. Specifically, controlling infection and bleeding during the critical neutropenic and thrombocytopenic phases was the limiting factor in successful treatment [22-24]. For example, in one study the LD50/30 value (ie, the radiation dose lethal to 50 percent of the study subjects in 30 days) in canines increased significantly from 2.6 Gy without supportive care to approximately 3.4 Gy following use of supportive care alone [25]. The LD50/30 was prolonged further to 5.5 Gy following the early addition of hematopoietic colony stimulating factors. Similar results have also been reported for non-human primates [26-32].
The mean lethal dose of radiation required to kill 50 percent of humans at 60 days (LD50/60) is a whole-body radiation dose between 3.25 to 4 Gy in persons managed without any supportive care, and 6 to 7 Gy when antibiotics and transfusion support are provided. Extrapolating from the survival benefit demonstrated in animal studies, the lethal dose may be somewhat higher with early initiation of colony stimulating factors. However, a whole-body dose >10 Gy is likely to be lethal.
Given the similarities between patients with the hematopoietic radiation injury syndrome and those undergoing hematopoietic cell transplantation, many of the fundamentals in supportive care, prophylaxis, blood product support, and infection management remain the same.
BLOOD PRODUCTS — Blood product support is required for patients with severe degrees of cytopenia resulting from radiation-induced bone marrow aplasia and for those with anemia secondary to gastrointestinal and other blood losses. Severe degrees of anemia and thrombocytopenia do not typically occur before two to four weeks following exposure, during which time a sufficient number of additional blood donors may be identified when there are large numbers of injured patients.
Irradiation of blood products — All cellular blood products should be irradiated (25 Gy) to prevent transfusion-associated graft-versus- host disease (TA-GVHD), a life threatening form of acute GVHD that occurs in immunosuppressed patients given blood products containing viable proliferating allogeneic lymphocytes.
TA-GVHD is almost uniformly fatal and may be difficult to distinguish from other organ toxicities seen in radiation victims (eg, fever, pancytopenia, skin rash, diarrhea, and abnormal liver function). Fortunately, this complication is fully preventable through the irradiation of cellular blood products.
Leukoreduction — Leukoreduction is known to lessen febrile nonhemolytic reactions and the immunosuppressive effects of blood transfusions [33,34]. It also affords some protection against platelet alloimmunization and cytomegalovirus infection [35]. However, leukoreduction alone is not sufficient to protect patients from transfusion-induced GVHD. Irradiation of all blood products is the only way to assure complete safety from the latter complication.
Accordingly, all blood products should be irradiated and, if possible, leukoreduced whenever time and facilities permit. However, when this is not possible, life-saving blood products should not be withheld.
Transfusion guidelines — Guidelines for transfusion of red cells and platelets should follow those recommended for patients recovering from chemotherapy (table 11 and table 12).
ASCO platelet transfusion guidelines - Part I
|
Platelet products: |
|
The benefits of pooled platelets or single donor platelets are similar; the two products can be used interchangeably. Single donor platelets from selected donors are preferred when histocompatible platelet transfusions (ie, HLA-A and HLA-B antigen matched) are needed. |
|
Prophylactic platelet transfusion thresholds: |
|
Acute leukemia: |
|
For adult patients, a threshold of 10,000/µL is recommended. Transfusion at higher levels may be necessary in the newborn, or in patients with hemorrhage, high fever, hyperleukocytosis, rapid fall in platelet count, or coagulation abnormalities. |
|
Hematopoietic cell transplantation: |
|
Same as for acute leukemia, with similar caveats. |
|
Chronic stable severe thrombocytopenia: |
|
Many patients can be observed without prophylactic transfusion, reserving transfusion for episodes of hemorrhage or during times of active treatment. |
|
Solid tumors: |
|
Evidence supports the benefit of prophylactic transfusion at a threshold of 10,000/µL or less. A threshold of 20,000/µL should be considered for patients receiving aggressive therapy for bladder cancer, as well as those with demonstrated necrotic tumors. |
|
Surgical or invasive procedures: |
|
A platelet count of 40 to 50,000/µL is sufficient to perform major invasive procedures safely, in the absence of associated coagulation abnormalities. Certain procedures, such as bone marrow aspiration/biopsy can be performed safely with counts <20,000/µL; lumbar puncture in children is safe at platelet counts >10,000/µL. |
Modified from: Schiffer, CA, et al. Platelet transfusion for patients with cancer: Clinical practice guidelines of the American Society of Clinical Oncology. J Clin Oncol 2001; 19:1519.
ASCO platelet transfusion guidelines - Part II
|
Prevention of RhD alloimmunization: |
|
RhD-negative children (especially girls) and women of child-bearing age should be considered for treatment with either the exclusive use of platelets from RhD-negative donors or via anti-D immunoprophylaxis. |
|
Prevention of alloimmunization using leukoreduced blood products: |
|
It is appropriate to provide leukoreduced blood products to patients with AML from the time of diagnosis to ameliorate the problem of alloantibody-mediated refractoriness to platelet transfusion. Currently, this is not indicated in patients with cancer receiving RBCs or treatments that do not produce significant and sustained thrombocytopenia. Universal leukoreduction of blood products would obviate the need for these decisions inindividual patients. |
|
Diagnosis of refractoriness to platelet transfusion: |
|
A corrected count increment (CCI) of ≥5,000 (see text for definitions) is recommended as a definition of a satisfactory response. A rough estimate of a CCI of 5,000 is an absolute platelet count increment of 2,000/µL per unit of platelet concentrate given to an average-sized adult. For children, an approximate equivalent is an absolute platelet count increment of 3,500/µL per meter squared per transfused unit. A diagnosis of refractoriness should be entertained only when at least two consecutive ABO-compatible transfusions, stored less than 72 hours, result in poor increments. |
|
Managment of refractoriness to platelet transfusion: |
|
Patients with alloimmune refractory thrombocytopenia (ie, poor increments in association with alloantibody detected using lymphocytotoxicity or antiplatelet antibody assays) are best managed with HLA-A and HLA-B antigen selected donors or from compatible donors identified using platelet cross matching techniques. Alloimmunized patients do not benefit from unmatched prophylactic platelet transfusions that fail to raise the platelet count. Such patients should be transfused only for hemorrhagic events. |
Modified from: Schiffer, CA, et al. Platelet transfusion for patients with cancer: Clinical practice guidelines of the American Society of Clinical Oncology. J Clin Oncol 2001; 19:1519.
Support with granulocyte transfusions may sometimes be useful for controlling refractory infections during the period of neutropenia, but as yet has not been formally evaluated in controlled trials of subjects with radiation injury. (See "Granulocyte transfusions", section on 'Minimal criteria'.)
CYTOKINES — Transient or permanent cytopenias after radiation exposure develop as a result of damage to bone marrow stem cells and progenitor cells. Depending on radiation dose, cytopenias may improve transiently, causing an "abortive rise" in the circulating neutrophil count (figure 1) or may inexorably progress. Hematopoietic recovery following radiotoxicity occurs through proliferation of:
- Undamaged stem/progenitor cells that escape from exposure due to inhomogeneously irradiated bone marrow [10]
- Relatively radioresistant stem/progenitor cells [36].
Whereas infusion of hematopoietic stem/progenitor cells is required to successfully treat irreversible cytopenias [37], cytokines may accelerate hematopoietic recovery in the case of reversible hematopoietic toxicity.
Neutrophil recovery — Studies in patients with cancer [38] and in a small number of radiation accident victims [39,40] have demonstrated an apparent beneficial effect of cytokines on neutrophil recovery in man. Controlled trials of cytokine therapy in mice, non-human primates, and canines have also shown improved survival after lethal irradiation [27,41,42].
Recommendations — None of the available cytokines has formal FDA approval for the management of radiation-induced aplasia of the bone marrow. Nevertheless, based upon results of studies in irradiated animals and an apparent shortening of the period of granulocytopenia in victims of radiation accidents, cytokines are recommended under some circumstances after radiation exposure.
Guidelines for use of cytokines in acute radiation injury have been developed in the United States [1] and Europe [43]. Expert opinion suggests that cytokines should be administered soon after (ie, within 24 hours) an exposure of >3Gy has occurred or when clinical signs and symptoms indicate a level 3 degree of hematotoxicity.
A lower threshold exposure dose (ie, 2 Gy) should be considered for initiation of cytokine therapy in children <12, adults >60, and individuals of any age who have mechanical injuries and/or thermal burns. All individuals with an absolute neutrophil count <500/microL should be considered for cytokine therapy.
Granulocyte-colony stimulating factor (G-CSF) at a dose of 5 microg/kg of body weight per day subcutaneously has been recommended as treatment in this setting. Other cytokines (eg, pegylated G-CSF or granulocyte-macrophage colony-stimulating factor (GM-CSF)) may be considered. Cytokine therapy should be continued for 2 to 3 weeks or until the absolute neutrophil count is >1000/microL.
Stimulation of erythropoiesis — The benefit of recombinant human erythropoietin or darbepoetin in this setting has not been established, but can be considered in patients with persistent anemia and a hematocrit <30 percent. A baseline serum erythropoietin level may be helpful, and supplementation with iron should be considered if these agents are employed. Clinical benefit may not be seen for three to six weeks.
ANTIBIOTICS — Susceptibility to local and systemic infection after radiation arises as a result of:
- Breeches in cutaneous and mucosal barriers
- Immune suppression and neutropenia
Background — Studies in irradiated mice have demonstrated that normal endogenous gut flora undergo a dose-related reduction in numbers within the first four days postradiation [17,44]. This is followed by a relative increase in the number of Enterobacteriaceae compared with anaerobic bacteria by the 12th day. Fatal bacteremia may then result from the bacterial translocation of these organisms. Quinolone use was effective in controlling systemic endogenous Gram-negative infections after radiation [45,46]. Supplementation with penicillin prevented treatment failures due to Streptococci and increased survival in animals. Quinolones given for 21 days were also effective in preventing endogenous Klebsiella and Pseudomonas infections in preclinical models [17,45,46].
Bacterial infection — Most infections during neutropenia caused by myelosuppressive chemotherapy or radiation treatment regimens are bacterial. The risk for life-threatening infection is particularly high when the absolute neutrophil count (ANC) is <100 cells/microL. As in animals, antibiotic prophylaxis provides a protective benefit that in meta-analyses has been associated with fewer infections, fewer bacteremic episodes, lower infection-related mortality, and improved survival [47].
While controversy exists over prophylaxis with the fluoroquinolones, their use has been explored extensively for prophylaxis in high-risk neutropenic patients and has demonstrated a reduction in the incidence of infectious episodes and bacteremic episodes [48-52], and in meta-analyses improved survival [47,53]. Consideration for their use should be given to patients with profound neutropenia (ie, ANC <100 cells/microL) expected to persist for >10 days.
Fever during neutropenia is most commonly due to a bacterial infection. In patients who experience neutropenic fever, the recommendations of consensus panels, such as the Infectious Diseases Society of America and National Comprehensive Cancer Network for evaluation and management are sensible guidelines [54,55]. For patients receiving fluoroquinolone prophylaxis, the fluoroquinolone should be stopped and the patient should undergo a prompt fever workup, including physical examination and blood cultures. Parenteral therapy, directed at gram-negative bacteria, and in particular, Pseudomonas aeruginosa, should be instituted urgently, as gram negative infections may be rapidly lethal.
This serves as the minimum backbone of antibiotic usage. Additional antimicrobials should be added to broaden coverage as clinically required to treat other foci of infection secondary to mucosal or integument injury.
The IDSA clinical practice guidelines for the use of antimicrobial agents in neutropenic patients with cancer, as well as other IDSA guidelines, can be accessed through the Infectious Diseases Society of America's web site [56].
Skin and respiratory bacteria may be important pathogens, more so than in the cancer patient, if there is significant injury to the integument or damage to respiratory mucosal epithelium by burns or inhalation of radioactive particulates. Antibiotics with coverage against Gram positive bacteria may need to be considered in such situations.
Fungal infection — Invasive Candida infections are the most frequent fungal pathogens in neutropenic patients. Fluconazole has been shown to lessen mucosal and invasive Candida fungal infections and fungal-related mortality in patients undergoing allogeneic hematopoietic cell transplantation [57,58] at doses of 200 to 400 mg by mouth daily. Data in patients receiving conventional forms of severely myelotoxic chemotherapy also have demonstrated benefits in using this agent [59], although conflicting results exist [60,61]. Fluconazole prophylaxis is ineffective against aspergillus, molds, Candida krusei, and resistant Candida species. Invasive infections by mould pathogens become increasingly more problematic when neutropenia persists for more than two weeks.
The opportunistic pathogen Pneumocystis jirovecii (formerly pneumocystis carinii) is classified as a fungus. It has unique tropism for the lungs, with rare dissemination. Patients with profound T-helper cell depletion (ie, absolute CD4 count <200/microL) are at risk for infection. Prophylaxis is warranted, given its associated high mortality, although no defined guidelines for monitoring of the CD4 count in irradiation patients exist.
However, extrapolating from the HIV and stem cell transplant experience, for patients who have survived a significant radiation exposure, the absolute CD4 count should be assessed at approximately day 30 post-exposure, and then every 3 to 6 months until the absolute CD4 count is >200/microL. Initiation and maintenance of prophylaxis is recommended if the absolute CD4 count is <200/microL. In patients with persistent myelosuppression, trimethoprim-sulfamethoxazole should be avoided as it may worsen existing cytopenias. Atovoquine, dapsone, and pentamidine are alternative agents. Discontinuation of prophylaxis can be considered when the absolute CD4 count is >200/microL.
Herpes simplex virus — Because of intense immunosuppression, patients with radiation injury are at risk for herpes simplex virus (HSV) reactivation, which may be confused with radiation stomatitis and may complicate its management by adding to the severity of mucosal injury [62].
Herpes simplex virus (HSV) serological status should be determined if resources allow, and prophylaxis should be employed, using acyclovir or valacyclovir in those who are serologically positive for HSV types I or II. Because of intense immunosuppression, these patients are at high risk for HSV reactivation, which may be confused with radiation stomatitis and may complicate its management by adding to the severity of mucosal injury [62].
If HSV serologies are not known, HSV prophylaxis can be reasonably offered based on any previous history of oral or genital herpes infections. Additionally, any patient not receiving prophylaxis and suffering from mucositis, especially if unusually severe or prolonged, should be assessed for possible HSV reactivation.
Cytomegalovirus — The incidence of reactivation of cytomegalovirus (CMV) in those patients harboring a latent CMV infection may be increased; the degree to which this causes CMV disease and its attendant mortality is unknown. If resources permit, CMV serologic status should be assessed. If the patient is CMV seronegative, blood products from CMV seronegative donors should be provided whenever possible. Alternatively, leukoreduced products provide a protective effect against transmission of CMV.
Because of this uncertainty, CMV antigen or PCR assessment should be performed weekly from approximately days 30 to 100 post-exposure. Frequently, detection of CMV in blood antedates disease by one to two weeks.
Patients with evidence of early CMV viremia should be treated preemptively, prior to the development of CMV disease, with either ganciclovir or valganciclovir. For those patients with a history of CMV reactivation and continued T-cell immunodeficiency (ie, CD4 count <50/microL), more protracted monitoring should be considered, such as every other week until 6 months post-exposure. Appropriate consultation with an Infectious Disease consultant followed by appropriate therapy should be instituted for those patients who develop CMV disease.
Other pathogens — It is anticipated that these patients will be at high risk for infection due to an enhanced susceptibility to many pathogens, including atypical fungi and other viruses. Some viral infections may be newly acquired and others may be due to reactivation. A high index of suspicion is required, especially in patients with culture negative fever and those with fever and pulmonary infiltrates.
Recommendations — For those who experience significant neutropenia (ie, absolute neutrophil count <500/microL), broad spectrum prophylactic antimicrobials should be employed, as the neutropenic duration is likely to be prolonged (table 9 and figure 1). Prophylaxis should include a fluoroquinolone (FQ) with streptococcal coverage (or penicillin or amoxicillin added to the FQ if it is not inherently covered by the FQ), an antiviral agent if the patient is herpes simplex virus (HSV) positive, and an antifungal agent.
These agents should be continued until the patient fails treatment, develops toxicity, experiences a neutropenic fever, or experiences neutrophil recovery (ANC >500/microL). Any foci of infection that develop during the neutropenic period will require a full course of antibiotic therapy.
In patients who experience neutropenic fever, therapy should follow the recommendations of the Infectious Diseases Society of America [55]. For patients receiving fluoroquinolone prophylaxis, the fluoroquinolone should be stopped and the patient should undergo a fever work-up. Parenteral therapy, directed at gram-negative bacteria, and in particular, Pseudomonas aeruginosa, is administered urgently, as gram negative infections may be rapidly lethal.
This serves as the minimum backbone of antibiotic usage. Additional microbials should be added to broaden coverage as clinically required to treat other foci of infection secondary to mucosal or integument injury [56].
HEMATOPOIETIC CELL TRANSPLANTATION
Historical perspective — The scientific basis for treatment with hematopoietic cell transplantation (HCT) was developed by demonstrating that experimental animals could be protected against lethal hematopoietic injury by intravenous infusion of bone marrow cells [63]. Given this background, it would seem obvious that HCT might be utilized to treat patients with severe bone marrow injury from a radiation overdose. However, the use of HCT in these patients is complicated by a variety of factors:
- Radiation exposure is often not homogeneous. For example, patients might have bone marrow ablative doses of radiation to parts of their body, but other marrow-containing structures might be minimally or unirradiated. This can come about because the patient was partially shielded by an automobile, desk, wall, or other barrier.
- Concomitant injuries such as burns or trauma can greatly complicate the care of patients who also have radiation-induced bone marrow failure. In a compilation of 58 patients who had potentially lethal radiation exposure, the major causes of deaths were burns (55 percent), hemorrhage (41 percent), infection (15 percent), and acute respiratory distress syndrome (15 percent) [64]. Obviously, HCT would not have repaired the vast majority of these fatal injuries.
- Explosion of a nuclear device leading to mass casualties would also destroy the infrastructure necessary to care for these patients. Losses would include not only hospital centers and supplies, but also medical, nursing, and ancillary personnel. The likelihood of identifying patients who might benefit from HCT seems slim when hospital beds and the necessary personnel to carry out sophisticated support services have also been damaged or destroyed.
Using HCT to treat radiation victims requires an accurate assessment of exposure. As an example, doses below 3 Gy would usually not be fatal if excellent nursing care was available, and the upper dose limit that can be survived without HCT might be in the range of 7 Gy following the prompt use of hematopoietic growth factors and aggressive supportive care. On the other hand, doses in excess of 10 Gy are likely to be fatal because of injury to organ systems other than bone marrow (eg, cerebrovascular and gastrointestinal). This leaves only a small fraction of patients who might benefit from HCT (ie, doses of 7 to 10 Gy for those receiving allogeneic HCT and 4 to 10 Gy for those able to receive autologous or syngeneic HCT).
Case selection — The most favorable situation would involve a patient who had fully compatible hematopoietic stem cells immediately available for an autologous hematopoietic cell transplantation. Examples include:
- Military personnel at high risk might have such cells stored for emergency purposes
- Patients may have stored stem cells as a potential backup treatment for a previously documented malignancy
- Patients may have their own umbilical cord blood in long-term storage.
- Patients with identical twins (syngeneic HCT)
It would seem wise to be liberal in the use of HCT to treat these patients and to err on the side of overutilization, since complications of either autologous or syngeneic HCT in this setting should be minimal.
However, it is unlikely that victims of radiation overexposure fall into any of the above settings or even know that they have an HLA matched sibling. It is even more unlikely that a patient would have had a recently completed search for a matched unrelated donor. The ability to carry out either of these activities after a radiation event depends upon the size of the event and the number of injured victims. However, it is possible that HLA typing of siblings or an accelerated search for an unrelated donor might be accomplished when the number of victims is small.
A haplotype-matched donor might be considered, especially in children. Unfortunately, available data on the treatment of radiation injury with allogeneic HCT are not encouraging:
- In 29 patients who underwent HCT after accidental radiation overdose, the median survival was only 33 days [64]. While all 29 patients had some evidence of engraftment (ie, 10 to 100 percent of bone marrow cells being of donor origin) 14 days post-transplant, there was no evidence for permanent engraftment in any of the survivors.
- All patients with burns died and only three patients survived for more than one year, two following infusion of bone marrow stem cells and one following use of fetal liver cells. It is impossible to determine whether or not their survival was related to the HCT, since no survivor had permanent donor engraftment.
- In 7 of the 29 patients (24 percent) graft-versus-host disease (GVHD) was felt to be a major contributing cause of death.
Similar results were observed in two radiation accidents in Japan, where two of three victims received allogeneic HCT [65]. One patient received a mismatched unrelated umbilical cord blood HCT and the other received a HLA identical sibling donor HCT [66]. Both transplanted patients demonstrated transient donor cell engraftment followed by autologous hematopoietic recovery before eventually dying of other radiation injuries.
Summary — It is difficult to be optimistic about a major contribution of HCT in the treatment of patients with radiation injury. The chance of identifying patients with lethal marrow injury, no lethal injury to other organs, no severe burns or trauma, and an intact medical infrastructure, seems poor. The prognosis for a transplant patient following radiation injury would be even worse if/when additional complications occur, such as infection and respiratory failure. In particular, a mass casualty situation requires an early estimation of prognosis in order to appropriately address available resources to those most likely to survive admission to an intensive care unit.
In the rare patient with a significant exposure (ie, 4 to 10 Gy) who might have an autologous or syngeneic HCT option, a stem cell infusion should be considered, as it would have low morbidity and would likely lead to earlier hematologic reconstitution, which might be lifesaving (table 9).
If resources allow, the use of a matched sibling or unrelated allogeneic HCT can be considered in the rare patient with a significant exposure (ie, 7 to 10 Gy), with minimal to no extramedullary injuries, and with a rapidly identified volunteer donor. Additional considerations should be given to the exploration of novel transplant methods (eg, non-myeloablative HCT) and stem cell sources (eg, umbilical cord blood HCT) in this small subset of irradiated victims deemed eligible for such treatment [67].
OTHER MEDICAL ISSUES
Immune reconstitution — Immune reconstitution in some patients will likely be aberrant and radiation dose-dependent, especially since single fraction total body irradiation (TBI) is more immunosuppressive than fractionated TBI [68].
Extrapolating from the transplantation literature, functional hyposplenism may occur following transplantation with total body irradiation-containing regimens. However, many of these patients had allogeneic HCT and also had chronic graft-versus-host disease. It is difficult to predict the extent to which radiation may affect splenic function, but it should be assessed as a potential long-term risk for those patients with a significant exposure who survive the event.
Accordingly, convalescent serologies should be assessed at one year following any significant whole body exposure.
Additionally, one should consider monitoring of immunoglobulin levels in these patients, especially in the presence of recurrent sinopulmonary infections.
Intravenous immunoglobulin is not ordinarily required in patients with reduced IgG levels unless recurrent sinopulmonary infections occur. In patients receiving intravenous immunoglobulin for longer than one year, delayed immune production of immunoglobulins may occur. Moreover, revaccination of patients who have received immunoglobulin replacement within three months may yield a suboptimal response.
Revaccination should follow the CDC/ASBMT/IDSA guidelines with the additional consideration of vaccination for polysaccharide encapsulated organisms such as Streptococcal pneumonia, Neisseria meningococcus, and Hemophilus influenzae type B if functional hyposplenism is suspected. Repeat serologies to assess vaccination efficacy is warranted.
The IDSA clinical practice guidelines for preventing opportunistic infections among HSCT recipients, as well as other IDSA guidelines, can be accessed through the Infectious Diseases Society of America's web site [56].
Immunization of unaffected family members can be useful to reduce the risk of exposure to infectious agents and provide some protection to the patient during the period before immunization is possible. The patient should avoid exposure to any individual who has received the oral polio vaccine, since transmission of virus is possible for weeks after the immunization. The inactivated polio vaccine is advisable for family members to avoid risk of transmission.
If a serologic response is not achieved, use of prophylactic penicillin V or another antibiotic with activity against encapsulated bacteria should be considered. Live vaccines should not be given until at least 24 months after exposure and should only be done in patients with some evidence of immune recovery. This may require consultation with an Immunologist.
There is a substantial clinical database showing that myelosuppressive chemotherapy or myeloablative conditioning prior to HCT has deleterious effects on immune recovery [69-71]. To date, there is no effective treatment for the prolonged T cell deficiencies associated with cytotoxic therapy. The significant delay in regeneration of CD4 + T cells, marked imbalance in the CD4/CD8 ratio, and a limited T-cell receptor repertoire leave the patient at risk for infectious complications.
Several cytokines, including the Interleukins (IL)-2, 4, 7, 17, c-kit ligand (KL), flt-3 (FL), thymic stromal lymphopoietin (TSLP), and keratinocyte growth factor (KGF) have been associated with T-cell differentiation, proliferation, and enhanced thymopoiesis and functional recovery of peripheral T cells in investigational studies, but there is no experience with their use in subjects with radiation injury [72-77]. This subject is explored in depth separately [21].
Internal contamination — Immediate skin and wound decontamination will eliminate or reduce uptake of radioactivity from these routes. However, organ doses from internal emitters are rarely high enough to cause the acute radiation syndrome. Accordingly, treatment decisions concerning internal contamination will primarily involve concerns about late health effects, such as radiation-induced carcinogenesis.
These treatment considerations should take into account the age and co-morbidities of the patient. For example, children are more radiosensitive than adults and have a longer life expectancy. In contrast, older patients with significant co-morbidities are less likely to benefit from treatment of internal contamination, as they may not live long enough to manifest long-term sequelae.
If radioactive isotopes of iodine are present, potassium iodide (KI) blockade of thyroid should be initiated immediately . Ideally, patients would already have KI present in their homes, with a priority of treatment directed toward those with the highest risk of subsequent development of thyroid cancer.
Any patient with evidence to suggest internal contamination (eg, by history, a positive nasal swab, or known wound contamination) should be examined to ascertain the principal radionuclides present consequent to the exposure. The metabolic behavior of the radionuclides present and their biologic significance can then be ascertained. This assessment should be undertaken with guidance from the radiation safety officer and may include examination of the radionuclide content in the excreta (urine and stool) and /or employment of a whole-body counter.
Goals of treatment are based on the radionuclides present and current knowledge of their clinical consequences. Treatment principles may include:
- Reduction and/or inhibition of absorption from the GI tract
- Blocking organ uptake (eg, potassium iodide)
- Employment of isotope dilution
- Alteration of the chemistry of the contaminating substance
- Displacement of the isotope from its receptors
- Employment of chelation
- Lung lavage
The table presents a brief overview of selected internal contaminants and their potential treatment (table 13). A number of excellent sources are available for clinical guidance on this subject. These include:
- NCRP 65: "Medical Management of Radiation Accidents" by I. Gusev, A. Guskova, F. Mettler, 2nd ed, 2001.
- The Radiation Emergency Assistance Center/Training Site (REAC/TS), www.orau.gov/reacts, has expertise in radiation injury, including internal contamination management. This Department of Energy asset also maintains a 24 hour emergency hotline: 1-865-576-1005 (ask for REAC/TS).
Treatment of selected internal radioactive contaminants
|
Contaminant |
Treatment |
Principal action(s) |
|
Americium |
Wound excision, Ca-DTPA or Zn-DTPA |
Chelation |
|
Californium |
||
|
Plutonium |
||
|
Curium |
||
|
Cerium |
||
|
Cesium |
Prussian Blue |
Accelerates removal |
|
Rubidium |
||
|
Thallium |
||
|
Iodine |
Potassium iodide |
Blocks thyroid uptake |
|
Strontium |
Aluminum antacids, ammonium chloride, calcium, barium sulfate, phosphate |
Blocks GI absorption, promotes urinary excretion and mobilization from bone |
|
Tritium |
Fluids, diuretics |
Dilutes the isotope and promotes diuresis |
|
Uranium |
Sodium bicarbonate |
Decreases uranyl nephrotoxicity |
DTPA: diethylenetriamine pentaacetate.
Revised from Gusev, I, Guskova, AK, Mettler, FA, eds. Medical management of radiation accidents, 2nd edition. CRC Press, Boca Raton, FL; 2001.
OVERALL RECOMMENDATIONS — Currently, there is only one treatment protocol for radiation-induced injury. The merits of good supportive care should not be underestimated, given the significant survival benefit observed in preclinical studies and in survivors of radiation accidents. The fundamentals of such management should include:
- Aggressive supportive care consisting of fluids, antibiotics, platelets, and other blood components. All cellular products require leukoreduction and irradiation.
- Administration of one of the granulopoietic cytokines, such as G-CSF, GM-CSF, or pegylated filgrastim should be considered as soon as possible following the exposure (table 14). However, even when employing pegylated G-CSF, standard G-CSF should be given daily for 3 to 5 days initially; the pegylated dose may be administered when chromosomal aberrations confirm the patient's exposure. Pegylated G-CSF has the convenience of a single injection, while daily G-CSF affords the ability to stop this agent if complications arise (eg, diffuse alveolar hemorrhage). Pegylated G-CSF is not approved in children weighing <45 kg.
- Immediately administer potassium iodide (initial adult dose: 130 mg PO) to those whose injuries resulted from a nuclear reactor accident or from a nuclear device detonation, and are therefore expected to have exposure to one or more radioactive isotopes of iodine (table 10). Priority administration should be given to children and pregnant females because of their unique circumstances and susceptibility to such exposures. The dose is continued daily until it is deemed safe to discontinue its use.
Cytokine doses after radiation exposure
|
Cytokine |
Adult dose* |
Precautions |
|
G-CSF |
5 µg/kg per day SQ until ANC >1000/microL |
Sickle cell disease, significant coronary art disease, ARDS• |
|
Pegylated G-CSF |
6 mg SQ as a single dose |
as with G-CSF |
|
GM-CSF |
250 µg/m2/day SQ until ANC >1000/microL |
as with G-CSF |
G-CSF: granulocyte colony-stimulating factor; GM-CSF: granulocyte-macrophage colony-stimulating factor; ARDS: acute respiratory distress syndrome; ANC: absolute neutrophil count.
* Recommended doses of G-CSF and GM-CSF are similar for adults, pregnant women, and children. Dose for pegylated G-CSF for adolescents >45 kg is the same as that for adults.
‧ Consider discontinuation of cytokines if pulmonary infiltrates develop at the time of neutrophil recovery.
Modified with permission from: Waselenko, JK, MacVittie, TJ, Blakely, WF, et al. Medical management of the acute radiation syndrome: Recommendations of the strategic national stockpile radiation working group. Ann Int Med 2004; 140:1039. Copyright c 2004 American College of Physicians.
DISASTER PLANNING AND ADDITIONAL RESOURCES — Beginning in 2001, the National Marrow Donor Program and the American Society for Blood and Marrow Transplantation established the Radiation Injury Treatment Network (RITN), a voluntary consortium of 52 transplant centers, donor centers, and umbilical cord blood banks [78]. The European Group for Blood and Marrow Transplantation is establishing a similar network [43,79].
The purpose of these networks is to develop treatment guidelines for managing hematologic toxicity among victims of radiation exposure [80], educate healthcare professionals about radiation exposure management, coordinate response after a radiation event, and provide evaluation and treatment for victims at participating transplant centers. Further guidance on the management of radiation exposure is available from the Oak Ridge Institute for Science and Education (ORISE) – Hospital triage and medical aspects of radiation incidents, including detailed procedure demonstrations for decontamination:http://www.orise.orau.gov/reacts/resources/default.aspx.
REFERENCES
10. Dainiak N. Hematologic consequences of exposure to ionizing radiation. Exp Hematol 2002; 30:513.
11. Sin, RC, et al. Biodosimetry assessment tool: a post-exposure software application for management of radiation accidents. Mil Med 2001; 166 (suppl 12):85.
13. Mental Health and Mass Violence, Evidence-Based Early Psychological Intervention for Victims/Survivors of Mass Violence. NIH Pub.02-5138. Washington, DC: National Institute of Mental Health Workshop; 2002.
14. Medical consequences of nuclear warfare. Walker, RI, Cerveny, RJ, eds. Office of the Surgeon General 1989. Available at www.afrri.usuhs.mil (Accessed 8/10/04).
15. Goans, RE. Clinical care of the radiation-accident patient: patient presentation, assessment, and initial diagnosis. In: Ricks, RC, Berger, ME, O'Hara, FM (Eds), The medical basis for radiation-accident preparedness: The clinical care of victims. Parthenon, Washington, DC 2002:11.
18. Additional information available at www.bt.cdc.gov/radiation/ki.asp (Accessed 8/10/04).
20. Accessed on June 8, 2009.
24. Sorensen, DK, Bond, VP, Cronkite, EP, Perman, V. An effective therapeutic regimen for the hemopoietic phase of the acute radiation syndrome in dogs. Radiation Res 1960; 13:669.
31. Stanley, RE, Seigneur, LJ, Strike, TA. The acute mortality response of monkeys (Macacca mulatta) to mixed gamma-neutron radiations and 250 kVp X rays.SR66-23. Bethesda, MD: Armed Forces Radiobiology Research Institute 1966.
33. Blajchman MA. Immunomodulation and blood transfusion. Am J Ther 2002; 9:389.
39. MacVittie, TJ, Farese, AM. Cytokine-based treatment for acute radiation-induced myelosuppression: preclinical and clinical perspective. In Ricks, RC, Berger, MD, O'Hara, F M Jr, eds. The medical Basis for Radiation Accident Preparedness. London: The Parthenon Publishing Group 2002; p. 53.
54. www.nccn.org (Accessed on October 12, 2010).
56. http://www.idsociety.org/Content.aspx?id=9088 (Accessed February 26, 2008).
62. Redding, SW. Role of herpes simplex virus reactivation in chemotherapy-induced oral mucositis. NCI Monogr 1990. p.103.
65. Maekawa, K. Overview of medical care for highly exposed victims in the Tokaimura accident. In: Ricks, RC, Berger, ME, O'Hara, FM (Eds), The medical basis for radiation accident preparedness. The clinical care of victims. Parthenon New York 2002. p.313.
80. www.ritn.net (Accessed on October 12, 2010).





 留言列表
留言列表
 線上藥物查詢
線上藥物查詢 