Volume 362:1804-1813
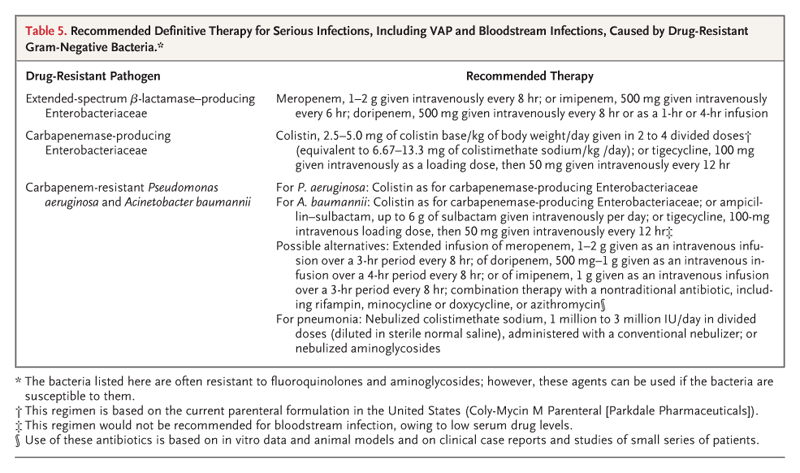
Figure 1. Mechanisms of Resistance in Gram-Negative Bacteria, and the Antibiotics Affected.
Seven mechanisms of resistance are shown in the gram-negative bacterium, with some being mediated by a mobile plasmid. These mechanisms include the loss of porins, which reduces the movement of drug through the cell membrane; the presence of β-lactamases in the periplasmic space, which degrades the β-lactam; increased expression of the transmembrane efflux pump, which expels the drug from the bacterium before it can have an effect; the presence of antibiotic-modifying enzymes, which make the antibiotic incapable of interacting with its target; target site mutations, which prevent the antibiotic from binding to its site of action; ribosomal mutations or modifications, which prevent the antibiotic from binding and inhibiting protein synthesis; metabolic bypass mechanisms, which use an alternative resistant enzyme to bypass the inhibitory effect of the antibiotic; and a mutation in the lipopolysaccharide, which renders the polymyxin class of antibiotics unable to bind this target. Red spheres indicate antibiotics.
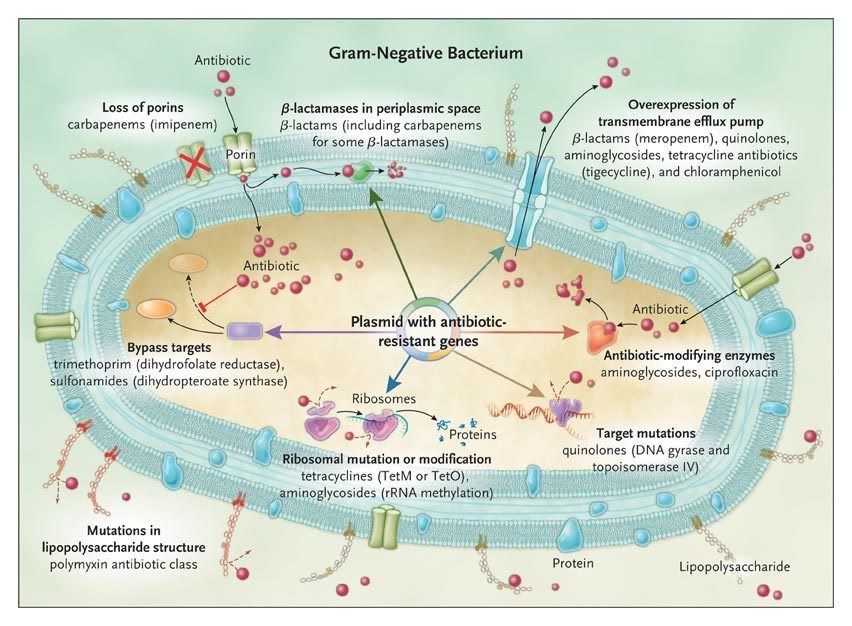
Table 1. Risk Factors for Health Care–Associated Infections and Infection with Drug-Resistant Bacteria.
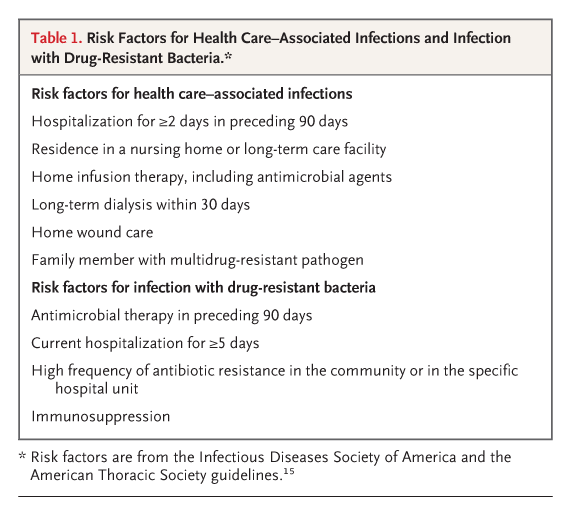
Table 2. Diagnostic Criteria and Management Guidelines for Ventilator-Associated Pneumonia

Table 3. Evidence-Based Guidelines for the Prevention of Hospital-Acquired Infections.
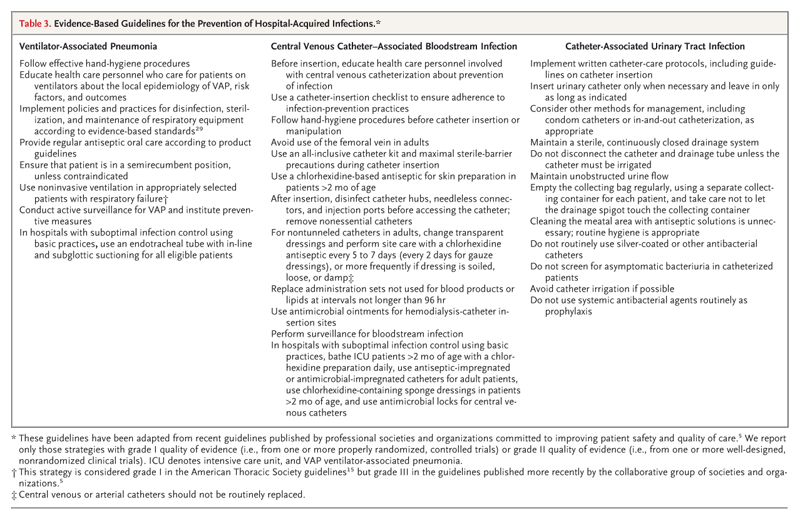
Table 4. Recommended Empirical Therapy to Cover Gram-Negative Organisms That Cause Hospital-Acquired Infections

Table 5. Recommended Definitive Therapy for Serious Infections, Including VAP and Bloodstream Infections, Caused by Drug-Resistant Gram-Negative Bacteria
如果你想多了解一點機轉,可以參考這邊:圖解藥理學~12抗生素機轉08





 留言列表
留言列表
 線上藥物查詢
線上藥物查詢 