日本最近的新聞真的是震撼到大家了,估且不提地震的緊急處理或是地震的緊急醫療,大型天災過後,應該要注意什麼呢?
首先,你應該要想到,跟水有關的天災,就要小心傳染病,再來就是地震受傷的,需要外傷護理,要是真的不幸有截肢的,還要注意殘肢痛(幻肢痛 phantom pain),
但是其實醫療不只醫病,還要醫心,所以我今天要跟大家介紹:創傷後壓力症候群post traumatic stress disorder
先寫一些中文描述,不然都沒有人要看了
創傷後壓力症候群的心理歷程
創傷後壓力症候群(PTSD)主要是一個人對於外來事件的一種心理生物學的反應,像是車禍、地震、被搶劫或性侵害等重大壓力事件都會使人產生PTSD。這些壓力必須是極度且相當突然的,並會造成強而有力的主觀反應,當事人經驗到強烈害怕、無助、驚恐。
下列現象是一般人在遭遇創傷事件後,經常會出現的反應,包括:
一、再經驗創傷事件:
不斷回想痛苦的記憶、情境再現(Flashbacks)、夢見創傷事件或其他的恐怖 事件、當回想到創傷事件時易引發過大的情緒和生理反應。
二、逃避:
逃避與創傷事件有關的活動、地點、思想、感覺。
三、情緒麻木:
對事物失去興趣、對人產生疏離感、情緒反應侷限。
四、警覺性增加:
睡眠困難、易被激怒、專注困難、過度警覺、驚嚇反應強烈。
若有上述情況,請不要害怕,這些都是自然且正常的反應,受影響較小的人會在短時間內自行恢復,有些人可能較嚴重,需要較長的時間與治療才能復原。有時候當事人會因為相關的身體化症狀而求助非精神科之醫療服務。
治療創傷後壓力症候群必須考慮許多方面,包括教育,支持,焦慮的處理,以及生活型態的重建。幫助當事人瞭解事實的真相,使其了解任何人在壓力之下都可能會產生創傷後壓力症候群。讓當事人接納災難已經發生過了,卸下再度去經驗創傷的重擔。鼓勵他們在團體中去分享經驗,並讓其知道有治療師、家人與朋友會一直支持他們,或參與長期性的支持團體效果更加。焦慮的處理技巧都可運用,可建議病人學習肌肉放鬆或接受呼吸訓練。生活型態的改變,例如:規則的睡眠、運動、維持健康的飲食都可以幫助病人重獲新生。
若你有親友有出現創傷症候群的話,你可以:
一、允許他說出對整著事件的描述。
二、支持與接受他表達情緒,允許他哭泣,甚至可以幫他說出他的心情,「你一定很難接受…」「你很遺憾來不及…」。
三、適切的肢體撫觸與擁抱。
四、協助他找到支持團體或有關的社會資源,必要時請心理專業機構或精神科協助。
INTRODUCTION — Post-traumatic stress disorder (PTSD) has been described as "the complex somatic, cognitive, affective and behavioral effects of psychological trauma" [1]. PTSD is characterized by intrusive thoughts, nightmares and flashbacks of past traumatic events, avoidance of reminders of trauma, hypervigilance, and sleep disturbance, all of which lead to considerable social, occupational, and interpersonal dysfunction.
The diagnosis of PTSD can be challenging because of the heterogeneity of the presentation and resistance on the part of the patient to discuss past trauma.
The diagnosis of PTSD is made in the subset of people who have experienced trauma who are unable to cope with the consequences of trauma and whose well-being over time is greatly impacted by these consequences. Concerns have been expressed about the potential to "over-medicalize" normal reactions to trauma, on one hand, while failing to recognize and address PTSD, on the other [2].
The treatment of PTSD is discussed separately.
EPIDEMIOLOGY — Many different types of trauma have been found to result in PTSD, including those listed below. Many of these events are common, resulting in a large number of affected individuals.
- Military combat
- Violent personal assault
- Natural and man-made disasters
- Severe motor vehicle accidents
- Rape
- Incest
- Childhood sexual abuse
- Diagnosis of a life-threatening illness
- Severe physical injury
- Hospitalization in an intensive care unit (ICU)
Prevalence and susceptibility — The lifetime prevalence of PTSD ranges from 6.8 to 12.3 percent in the general adult population in the United States (US) [3-5], with one-year prevalence rates of 3.5 to 6 percent [3,6,7]. In a study of 368 patients from a community primary care clinic, 65 percent reported a history of exposure to severe, potentially traumatic events; 12 percent went on to develop PTSD [8].
Personal and societal factors appear to affect both the likelihood of developing PTSD after a traumatic event and the clinical presentation of PTSD [2,9]. Risk factors for PTSD include lower socioeconomic status, parental neglect, family or personal history of a psychiatric condition, poor social support, and initial severity of reaction to the traumatic event [10-12]. In a study of male patients treated in primary care, Veterans Administration (VA) practices, 36 percent of patients who had been diagnosed with major depression screened positive for PTSD [13].
Trauma exposure and PTSD have also been associated with physical illness [14]. In a population-based study of 3171 community respondents, PTSD was associated with increased risks for angina (OR 2.4, 95% CI 1.3, 4.5), heart failure (OR 3.4, 95% CI 1.9, 6.0), bronchitis, asthma, liver, and peripheral arterial disease (ORs range = 2.5, 3.1) after adjusting for sociodemographic factors, smoking, body mass index, blood pressure, depression, and alcohol use disorders [14].
The frequency with which PTSD occurs after a traumatic event is influenced by characteristics of the individual and the inciting event [15]. Overall, women are four times more likely to develop PTSD than men, after adjusting for exposure to traumatic events [10]. The rates of PTSD are similar among men and women after events such as accidents (6.3 versus 8.8 percent), natural disasters (3.7 versus 5.4 percent), or sudden death of a loved one (12.6 versus 16.2 percent). Although women are more than 10 times as likely as men to be raped, the incidence of PTSD after rape is higher in men (65 versus 46 percent). The rate of PTSD is lower in men than in women after events such as molestation (12.2 versus 26.5 percent) and physical assault (1.8 versus 21.3 percent).
Higher rates of PTSD have been found in subgroups in the US compared to the general population, including Native Americans living on reservations and refugees from countries where traumatic stress was endemic. In two large samples of Native Americans, lifetime prevalence of PTSD ranged from 14.2 to 16.1 percent [16]. Among Cambodian refugees two decades after resettling in the US, 62 percent met criteria for PTSD in the last year [17].
Sexual assault — Sexual assault is the most frequent type of trauma experienced by women with PTSD [3,18]. In a nationally representative sample of 4,008 women in the United States (US), the lifetime prevalence of PTSD was 12.3 percent. Of the women who had a history of PTSD, 32 percent had been raped and 31 percent experienced a sexual assault other than rape [3].
Mass conflict and displacement — A meta-analysis of 145 studies of 64,332 refugees and other conflict-affected individuals internationally found a mean PTSD prevalence rate of 30.6 percent (95% CI, 26.3 - 35.2 percent) [19]. Factors associated with higher PTSD rates included reported torture, cumulative exposure to potentially traumatic events, shorter time since conflict, and the assessed level of political terror.
Combat — PTSD occurring after combat injury appears to be strongly correlated with the extent of injury, and develops over several months [20]. Rates of a positive screen for PTSD were higher when US veterans were surveyed three to six months following return from active duty, compared to results of surveys immediately on return [21]. In addition, up to 60 percent of returning soldiers with a positive PTSD screen on their initial survey reported symptom improvement by three to six months.
In another study of US soldiers hospitalized for war-related injuries, the prevalence of PTSD was 4.2 percent at one month and 12.2 percent by four months post-injury. Soldiers with a high severity of physical problems a month after injury were at greater risk of PTSD six months later, compared to those with lower physical problem severity (OR 7.0, 95% CI 3.1-16.0). Almost one-half of soldiers with war-related mild traumatic brain injury (concussion syndrome) met criteria for PTSD in one study; ongoing symptoms that had been attributed to direct effects of the brain injury may in fact relate to PTSD and be amenable to appropriate treatment [22].
War-related PTSD has been associated with long-term consequences for mental health [23]. A longitudinal cohort study compared a random sample of 450 Australian Vietnam veterans with matched subjects from the Australian general population. When assessed 36 years after the war, veterans with war-related PTSD were more likely than members of the general population to have depression, an anxiety disorder (eg, social phobia, panic disorder, agoraphobia with or without panic disorder, and specific blood phobia), alcohol dependence, or persistent pain disorder.
ICU hospitalization — A systematic analysis of 15 studies found the prevalence of PTSD in patients who survived intensive care unit (ICU) hospitalization to be approximately 20 percent [24]. Predictors of PTSD included prior psychopathology and greater use of benzodiazepines in the ICU; severity of critical illness was not a predictor of PTSD.
Cost — Extensive analyses of the cost of PTSD are rare, but suggest that PTSD is associated with increased health care costs and other direct and indirect costs. One study that looked at women with PTSD in a health maintenance organization (HMO) found that compared with women with few symptoms of PTSD, women with moderate and severe PTSD symptoms had increased median annual health care costs (38 and 104 percent higher, respectively) [25]. Exposure to trauma itself appears to be extremely costly in terms of the impact upon victims and their families and upon society. In one study, for example, severely victimized women in an HMO setting had medical expenses twice that of controls [26]. Other reports have estimated direct annual costs of personal crime in the US nationally to be $105 billion (medical costs, lost earnings, victim assistance programs); that figure increases to $450 billion annually when intangible losses (pain, suffering, quality of life) are considered [27].
PATHOPHYSIOLOGY — While much of the pathophysiology of PTSD is unclear, interesting research findings are accruing. Studies using MRI scans have shown that there is decreased volume of the hippocampus, left amygdala, and anterior cingulate cortex in patients with PTSD compared with matched controls [28,29]. Other reports have demonstrated increased central norepinephrine levels with down-regulated central adrenergic receptors [30], chronically decreased glucocorticoid levels with up-regulation of their receptors (possibly accounting for the anecdotal finding that there are more autoimmune diseases in these patients), and hemispheric lateralization in which there is a relative failure of left hemispheric function (possibly accounting for confusion related to time sequence of traumatic events) [31].
Researchers suspect that genetics may contribute to an individual's susceptibility to PTSD through an interaction with environmental factors [32]. However, research studies on the genetics of PTSD have generally been small and findings have been inconclusive [33]. As an example of a potential gene-environment interaction, the presence of one of four polymorphisms at the stress-related gene FKBP5 was found to be associated with an increased risk for PTSD in patients with a history of child abuse, but not in patients without history of child abuse [34].
Previous exposure to trauma appears to increase the risk of developing PTSD with subsequent traumatic events [35]. The mechanism by which this "sensitization" occurs is unclear. A study of severely injured accident victims who were healthy before experiencing trauma found that the incidence of PTSD was low [36].
CLINICAL MANIFESTATIONS — Most individuals who experience trauma react to some degree when experiencing reminders of the trauma. Patients with PTSD, however, experience marked cognitive, affective, and behavioral responses to stimuli, leading to flashbacks, severe anxiety, and fleeing or combative behavior. These individuals compensate for such intense arousal by attempting to avoid experiences that may begin to elicit symptoms; this can result in emotional numbing, diminished interest in everyday activities and, in the extreme, may result in detachment from others.
There are important distinguishing characteristics of PTSD symptoms in patients who experienced most of their trauma in childhood (eg, physical and sexual abuse) [1]. Compared with controls, these individuals often show greater difficulty with affect regulation (eg, unmodulated anger), and often demonstrate more dissociation, somatization, self-destructive behavior, and suicidal behavior.
Co-occurring conditions — Psychiatric comorbidity is high in patients with PTSD. The National Comorbidity Survey data suggests that 16 percent have one coexisting psychiatric disorder, 17 percent have two psychiatric disorders, and 50 percent have three or more [4]. Depressive disorders, anxiety disorders, and substance abuse are two to four times more prevalent in patients with PTSD; substance abuse is often due to the patient's attempts to self-medicate symptoms [4].
Traumatic brain injury (TBI) and PTSD have high rates of co-occurrence among civilians and, particularly, among soldiers who suffer combat-related TBI [37]. As an example, 11 percent of American soldiers returning from combat in Iraq and Afghanistan were reported to screen positive for PTSD in 2008. Among returning soldiers with mild TBI, 62 percent screened positive for PTSD [38].
Studies suggest that somatization disorder is as much as 90 times more likely in patients with PTSD than in patients without the disorder [39].
Course — Most individuals who develop PTSD experience its onset within a few months of the traumatic event. However, epidemiologic studies have found that approximately 25 percent experience a delayed onset after six months or more [40].
PTSD is commonly a chronic condition with only one-third of patients recovering at one year follow-up, and one-third still symptomatic ten years after the exposure to the trauma [4]. Individuals with one or more PTSD symptoms are more likely to experience marital difficulties and occupational problems, have poorer social supports, and have more disability than controls [41]. Additionally, PTSD may increase the risk for attempted suicide [42,43]
DIAGNOSIS — Patients presenting with symptoms of PTSD should receive a comprehensive psychiatric assessment. A diagnosis of PTSD is made for patients who meet all of the criteria below from the Diagnostic and Statistical Manual of Mental Disorders (DSM-IV-TR; (table 1) [44].
Criterion A: The person has been exposed to a traumatic event in which both of the following were present:
1. The person experienced, witnessed or was confronted with an event or events that involved actual or threatened death or serious injury, or a threat to the physical integrity of self or others.
2. The person's response involved intense fear, helplessness or horror. Note: in children this may be expressed instead by disorganized or agitated behavior.
Criterion B: The traumatic event is persistently reexperienced in one (or more) of the following ways:
1. Recurrent and intrusive distressing recollections of the event, including images, thoughts, or perceptions. Note: in young children, repetitive play may occur in which themes or aspects of the trauma are expressed.
2. Recurrent distressing dreams of the event. Note: in children there may be frightening dreams without recognizable content.
3. Acting or feeling as if the traumatic event were recurring (including a sense of reliving the experience, illusions, hallucinations and dissociative flashback episodes, including those that occur on wakening or when intoxicated). Note: in young children trauma-specific reenactment may occur.
4. Intense psychological distress and/or physiological reactivity on exposure to internal or external cues that symbolize or resemble an aspect of the traumatic event.
Criterion C: Persistent avoidance of stimuli associated with the trauma and numbing of general responsiveness (not present before the trauma), as indicated by three (or more) of the following:
1. Efforts to avoid thoughts, feelings or conversations associated with the trauma
2. Efforts to avoid activities, places or people that arouse recollections of the trauma
3. Inability to recall an important aspect of the trauma
4. Markedly diminished interest in participating in significant activities
5. Feeling detached or estranged from others
6. Restricted range of effect (eg, unable to have loving feelings)
7. Sense of a foreshortened future (eg, does not expect to have a career, marriage, children, or a normal life span)
Criterion D: Persistent symptoms of increased arousal (not present before trauma), as indicated by two (or more) of the following:
1. Difficulty falling or staying asleep
2. Irritability or outbursts of anger
3. Difficulty concentrating
4. Hypervigilance
5. Exaggerated startle response
Criterion E: Duration of the disturbance (symptoms in criteria B, C, and D) is more than one month.
Criterion F: Disturbance causes clinically significant distress or impairment in social, occupational, or other important areas of functioning.
Specify if:
Acute: if duration of symptoms is less than three months
Chronic: if duration of symptoms is three months or more
With delayed onset: if onset of symptoms is at least six months after the stressor
Adapted from Diagnostic and Statistical Manual of Mental Disorders, 4th ed, American Psychiatric Association, Washington, DC 1994.
- A severe, traumatic event causing intense fear or helplessness
- Resulting symptoms in each of three categories
- - Reexperiencing
- - Avoidance
- - Arousal
- Social or occupational impairment
- Symptoms and functional impairment lasting more than one month after the trauma
Examples of questions a clinician can ask to elicit symptoms are provided below.
- How do you feel when you recall the event?
- Do you experience dreams or flashbacks about it?
- Do you find yourself avoiding people or activities you associate with the event?
- Do you find yourself forgetting occurrences from that period?
- Do you find yourself looking carefully around when you are in a public place?
Patients need to be asked specific questions about their traumatic experience(s) to differentiate PTSD from other psychiatric disorders. These questions should be asked with sensitivity. Patients are often reluctant to discuss past traumatic events because of guilt, embarrassment, or discomfort inherent in revisiting painful memories.
Patients may minimize their symptoms of PTSD. Some patients may feel that past trauma has little or no effect on present symptoms. Military personnel in the US have been reported to be reluctant to disclose PTSD symptoms due to stigmatization and fear of professional repercussions [45].
Patients diagnosed with PTSD should also be assessed for suicidal or parasuicidal ideation or acts and co-occurring psychiatric conditions, substance use disorders, and medical conditions.
Instruments for screening and monitoring — In screening patients for PTSD, eg, primary care patients, returning veterans, or individuals experiencing domestic violence, particular attention should be paid to individuals presenting with new anxiety, fear, or insomnia [46]. Furthermore, clinicians may want to pay attention to associated behaviors in individuals at risk for PTSD anxiety symptoms, such as social isolation, increased substance abuse (alcohol and/or tobacco), or attempts at distraction through excessive work.
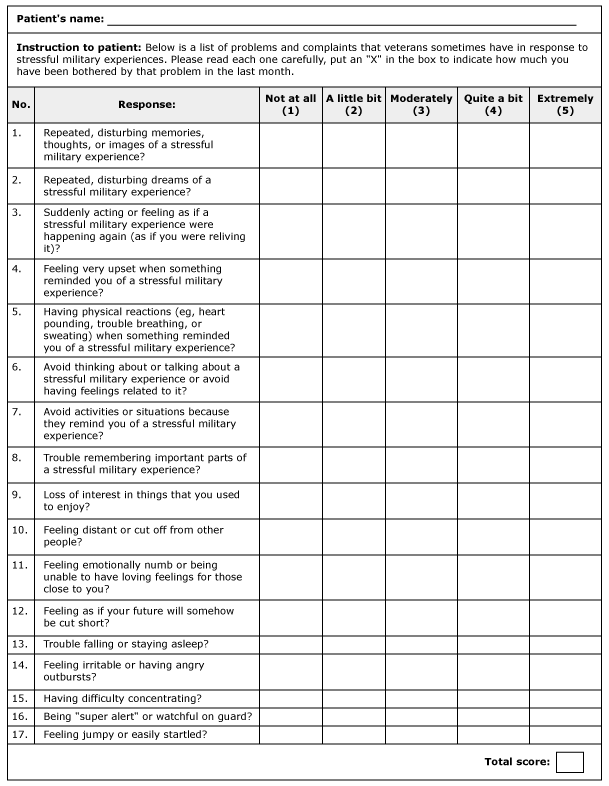
The PTSD checklist (PCL) may be helpful in screening patients for PTSD and monitoring the progress of treatment over time [47]. Versions of this tool have been developed for civilian and military populations (figure 1 and figure 2). For differing populations, the sensitivity of the PCL ranges from .69 to .94 and the specificity is from .83 to .99 [48-50]. A score of 50 out of a maximum score of 85 is associated with a diagnosis of PTSD. While the PCL is self-administered by patients, another option for assessing severity is the Clinician-Administered PTSD Scale (CAPS) [51].

Differentiating acute stress disorder — Individuals presenting with symptoms of post-traumatic stress and functional impairment after a highly traumatic event are diagnosed as having acute stress disorder (ASD) for the first 30 days following the event. Most people recover completely within this period. For those who remain symptomatic (at the threshold established by DSM-IV-TR criteria), their diagnosis is then reclassified as PTSD.
SUMMARY AND RECOMMENDATIONS
- The one-year prevalence of PTSD ranges from 3.5 to 6 percent in the US general adult population.
- Many different types of trauma can result in PTSD, including military combat, sexual or physical assault, disasters, childhood sexual abuse, severe physical injury, and ICU hospitalization.
- The pathophysiology of PTSD is not well understood. However, differences in neuroanatomy, neurotransmitters, and brain functioning have been found in individuals with the disorder.
- Individuals with PTSD experience marked cognitive, affective, and behavioral responses to stimuli reminding them of trauma they experienced, eg, flashbacks, severe anxiety, and fleeing or combative behavior. They compensate for this intense arousal through avoidance, emotional numbing, and diminished interest in people and activities.
- PTSD is commonly accompanied by comorbid psychiatric conditions, including depression, substance use disorders, and somatization.
- Diagnostic criteria for PTSD include: experiencing a severe, traumatic event causing intense fear; resulting symptoms in each of three categories (reexperiencing trauma, avoiding trauma-associated stimuli, and increased arousal); social or occupational impairment; and symptoms and impairment lasting at least one month after the trauma (table 1).
- A diagnosis of PTSD is made only after a month has passed since the traumatic event. Prior to that time, patients with PTSD-like symptoms and functional impairment are diagnosed with acute stress disorder.
REFERENCES
- van der Kolk, BA, Pelcovitz, D, Roth, S, et al. Dissociation, somatization, and affect dysregulation: the complexity of adaptation of trauma. Am J Psychiatry 1996; 153:83.
- Stein, DJ, Seedat, S, Iversen, A, Wessely, S. Post-traumatic stress disorder: medicine and politics. Lancet 2007; 369:139.
- Resnick, HS, Kilpatrick, DG, Dansky, BS, et al. Prevalence of civilian trauma and posttraumatic stress disorder in a representative national sample of women. J Consult Clin Psychol 1993; 61:984.
- Kessler, RC, Sonnega, A, Bromet, E, et al. Posttraumatic stress disorder in the National Comorbidity Survey. Arch Gen Psychiatry 1995; 52:1048.
- Kessler, RC, Chiu, WT, Demler, O, et al. Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry 2005; 62:617.
- Norris, FH. Epidemiology of trauma: frequency and impact of different potentially traumatic events on different demographic groups. J Consult Clin Psychol 1992; 60:409.
- Kessler, RC, Berglund, P, Demler, O, et al. Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry 2005; 62:593.
- Stein, MB, McQuaid, JR, Pedrelli, P, et al. Posttraumatic stress disorder in the primary care medical setting. Gen Hosp Psychiatry 2000; 22:261.
- Kroll, J. Posttraumatic symptoms and the complexity of responses to trauma. JAMA 2003; 290:667.
- Vieweg, WV, Julius, DA, Fernandez, A, et al. Posttraumatic stress disorder: clinical features, pathophysiology, and treatment. Am J Med 2006; 119:383.
- Liebschutz, J, Saitz, R, Brower, V, et al. PTSD in urban primary care: high prevalence and low physician recognition. J Gen Intern Med 2007; 22:719.
- Bisson, JI. Post-traumatic stress disorder. BMJ 2007; 334:789.
- Campbell, DG, Felker, BL, Liu, CF, et al. Prevalence of depression-PTSD comorbidity: implications for clinical practice guidelines and primary care-based interventions. J Gen Intern Med 2007; 22:711.
- Spitzer, C, Barnow, S, Völzke, H, et al. Trauma, posttraumatic stress disorder, and physical illness: findings from the general population. Psychosom Med 2009; 71:1012.
- Yehuda, R. Post-traumatic stress disorder. N Engl J Med 2002; 346:108.
- Beals, S. M. Manson, N. R. Whitesell, P. Spicer, D. K. Novins, and C. M. Mitchell. Prevalence of DSM-IV disorders and attendant help-seeking in 2 American Indian reservation populations. Arch Gen Psychiatry 2005; 62:99.
- G. N. Marshall, T. L. Schell, M. N. Elliott, S. M. Berthold, and C. A. Chun. Mental health of Cambodian refugees 2 decades after resettlement in the United States. JAMA 2005; 294:571.
- Chivers-Wilson, KA. Sexual assault and posttraumatic stress disorder: a review of the biological, psychological and sociological factors and treatments. Mcgill J Med 2006; 9:111.
- Steel, Z, Chey, T, Silove, D, et al. Association of torture and other potentially traumatic events with mental health outcomes among populations exposed to mass conflict and displacement: a systematic review and meta-analysis. JAMA 2009; 302:537.
- Grieger, TA, Cozza, SJ, Ursano, RJ, et al. Posttraumatic stress disorder and depression in battle-injured soldiers. Am J Psychiatry 2006; 163:1777.
- Milliken, CS, Auchterlonie, JL, Hoge, CW. Longitudinal assessment of mental health problems among active and reserve component soldiers returning from the Iraq war. JAMA 2007; 298:2141.
- Hoge, CW, McGurk, D, Thomas, JL, et al. Mild traumatic brain injury in U.S. Soldiers returning from Iraq. N Engl J Med 2008; 358:453.
- O'Toole, BI, Catts, SV, Outram, S, et al. The physical and mental health of Australian Vietnam veterans 3 decades after the war and its relation to military service, combat, and post-traumatic stress disorder. Am J Epidemiol 2009; 170:318.
- Davydow, DS, Gifford, JM, Desai, SV, et al. Posttraumatic stress disorder in general intensive care unit survivors: a systematic review. Gen Hosp Psychiatry 2008; 30:421.
- Walker, EA, Katon, W, Russo, J, et al. Health care costs associated with posttraumatic stress disorder symptoms in women. Arch Gen Psychiatry 2003; 60:369.
- Koss, MP, Woodruff, WJ, Koss, PG. Criminal victimization among primary care medical patients: prevalence, incidence, and physician usage. Behav Sci Law 1991; 9:85.
- Miller, TR, Cohen, MA, Wiersma, B. Victim costs and consequences: A new look. United States Department of Justice, National Institute of Justice, Research Report, Washington, DC 1996.
- Bremner, JD, Randall, P, Scott, TM, et al. MRI-based measurement of hippocampal volume in patients with combat-related posttraumatic stress disorder. Am J Psychiatry 1995; 152:973.
- Karl, A, Schaefer, M, Malta, LS, et al. A meta-analysis of structural brain abnormalities in PTSD. Neurosci Biobehav Rev 2006; 30:1004.
- Geracioti TD, Jr, Baker, DG, Ekhator, NN, et al. CSF norepinephrine concentrations in posttraumatic stress disorder. Am J Psychiatry 2001; 158:1227.
- van der Kolk, BA. The psychobiology of posttraumatic stress disorder. J Clin Psychiatry 1997; 58 Suppl 9:16.
- Kilpatrick, DG, Koenen, KC, Ruggiero, KJ, et al. The serotonin transporter genotype and social support and moderation of posttraumatic stress disorder and depression in hurricane-exposed adults. Am J Psychiatry 2007; 164:1693.
- Broekman, BF, Olff, M, Boer, F. The genetic background to PTSD. Neurosci Biobehav Rev 2007; 31:348.
- Binder, EB, Bradley, RG, Liu, W, et al. Association of FKBP5 polymorphisms and childhood abuse with risk of posttraumatic stress disorder symptoms in adults. JAMA 2008; 299:1291.
- Breslau, N, Chilcoat, HD, Kessler, RC, Davis, GC. Previous exposure to trauma and PTSD effects of subsequent trauma: results from the Detroit Area Survey of Trauma. Am J Psychiatry 1999; 156:902.
- Schnyder, U, Moergeli, H, Klaghofer, R, Buddeberg, C. Incidence and prediction of posttraumatic stress disorder symptoms in severely injured accident victims. Am J Psychiatry 2001; 158:594.
- Halbauer, JD, Ashford, JW, Zeitzer, JM, et al. Neuropsychiatric diagnosis and management of chronic sequelae of war-related mild to moderate traumatic brain injury. J Rehabil Res Dev 2009; 46:757.
- Schneiderman, AI, Braver, ER, Kang, HK. Understanding sequelae of injury mechanisms and mild traumatic brain injury incurred during the conflicts in Iraq and Afghanistan: persistent postconcussive symptoms and posttraumatic stress disorder. Am J Epidemiol 2008; 167:1446.
- Davidson, JR, Hughes, D, Blazer, DG, George, LK. Post-traumatic stress disorder in the community: an epidemiological study. Psychol Med 1991; 21:713.
- Smid, GE, Mooren, TT, van der Mast, RC, et al. Delayed posttraumatic stress disorder: systematic review, meta-analysis, and meta-regression analysis of prospective studies. J Clin Psychiatry 2009; 70:1572.
- Amaya-Jackson, et al. (unpublished data) cited in: Solomon, SD, Davidson, JRT. Trauma: Prevalence, impairment, service use, and cost. J Clin Psychiatry 1997; 58:5.
- Wilcox, HC, Storr, CL, Breslau, N. Posttraumatic stress disorder and suicide attempts in a community sample of urban american young adults. Arch Gen Psychiatry 2009; 66:305.
- Bernal, M, Haro, JM, Bernert, S, et al. Risk factors for suicidality in Europe: results from the ESEMED study. J Affect Disord 2007; 101:27.
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 4th ed, Text Revision, American Psychiatric Association, Washington, DC 2000.
- Hoge, CW, Castro, CA, Messer, SC, et al. Combat duty in Iraq and Afghanistan, mental health problems, and barriers to care. N Engl J Med 2004; 351:13.
- Wilson, JF. Posttraumatic stress disorder needs to be recognized in primary care. Ann Intern Med 2007; 146:617.
- Weathers, FW, Juska, JA, Keane, TM. The PTSD checklist - civilian version. Boston National Center for PTSD. Boston Veterans Affairs Medical Center 1991.
- Blanchard, EB, Jones-Alexander, J, Buckley, TC, Forneris, CA. Psychometric properties of the PTSD Checklist (PCL). Behav Res Ther 1996; 34:669.
- Weathers, FW, Huska, JA, Keane, TM. The PTSD Checklist Civilian Version (PCL-C) Boston, MA: National Center for PTSD (Boston Veterans Affairs Medical Center.1991.
- Andrykowski, MA, Cordova, MJ, Studts, JL, Miller, TW. Posttraumatic stress disorder after treatment for breast cancer: prevalence of diagnosis and use of the PTSD Checklist-Civilian Version (PCL-C) as a screening instrument. J Consult Clin Psychol 1998; 66:586.
- Blake, DD, Weathers, FW, Nagy, LM, et al. The development of a Clinician-Administered PTSD Scale. J Trauma Stress 1995; 8:75.





 留言列表
留言列表
 線上藥物查詢
線上藥物查詢 