BMJ 2012;345:e4955
[Link to free BMJ article PDF | PubMed® abstract]
類似的請參考:[US pharmacist]Complications of Cellulitis in Diabetic Foot Infections
Clinical Review
Diagnosis and management of cellulitis
Gokulan Phoenix, Saroj Das, Meera Joshi
Correspondence to: G Phoenix gokulan.phoenix@nhs.net
[EXCERPTS]
What causes cellulitis?
Table 1 Treatment recommendations for cellulitis based on organisms [Excerpts]
A prospective study demonstrated that the majority of S aureus infections in the US are now [methicillin] resistant; among 389 blood culture isolates of S aureus, 63% (244) were [community acquired]-MRSA.
A multicentre study of 11 US hospitals reported a prevalence of MRSA ranging from 15% to 74% (59% overall).
How is the diagnosis of cellulitis made?
Clinical diagnosis
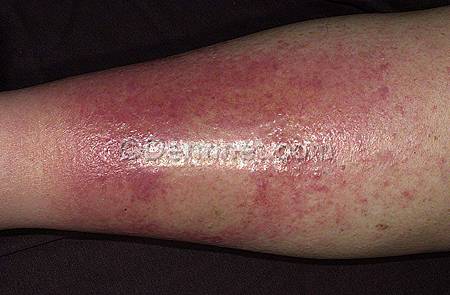
Cellulitis most commonly affects the lower extremities, and often presents as an acute, tender, erythematous, and swollen area of skin. In severe cases blisters, ulcers, oedema, associated lymphangitis, and lymphadenopathy may be present. Constitutional features include fever and malaise. In the late stages widespread features of sepsis including hypotension and tachycardia may also be present.
Blood investigations
An elevated level of C reactive protein is a better indicator of bacterial infection than an elevated white cell count but a normal level of C reactive protein cannot rule out an infection. Blood investigations do not appear to be clinically useful for diagnosis.
Microbiology
Prospective studies have shown true positive rates from blood cultures in those with suspected cellulitis are between 2-4%. The authors concluded blood cultures were neither clinically effective or cost effective. National guidelines, including the Northern Ireland Clinical Resource Efficiency Support Team (CREST) 2005 guidelines on the management of cellulitis in adults, recommend taking blood cultures only in patients that have significant systemic upset including pyrexia (>38°C).
In a prospective study of 50 patients with cellulitis, cultures from skin biopsies and aspirations that showed true positives were found to be 20% and 10% respectively. CREST guidelines suggest the use of skin biopsies and aspirations in only selected patients, where the diagnosis of cellulitis is in doubt.
In regard to wound swabs, a multicentre prospective study from France that analysed wound swab samples from 214 patients with lower limb cellulitis identified 183 (85.5%) positive cultures; S aureus and Streptococcus being the most frequently isolated micro-organisms (56% and 21% respectively). Sensitivities from the swabs showed resistance to the empirical antibiotics that had initially been used, prompting a change in antibiotics. CREST guidelines suggest the use of swabs on open cellulitis wounds.
Imaging
Imaging techniques are useful when there is a suspicion of an underlying abscess associated with cellulitis, necrotising fasciitis, or when the diagnosis of cellulitis is uncertain. In a retrospective study of 542 emergency department patients for whom the clinical diagnosis of cellulitis was in doubt, 109 (17%) were found to have a deep vein thrombosis on Doppler ultrasound.
Ultrasound may therefore guide management of cellulitis by detection of occult abscess, prevention of invasive procedures, and providing guidance for further imaging or consultation.
What is the treatment of cellulitis?
General measures include rest, elevation of any affected limbs, and analgesia. The area of cellulitis should be clearly marked and reviewed daily for progression or regression to assess the efficacy of the antibiotic regimen.
However, there is still uncertainty regarding the optimal antibiotic choice, duration, and route of antibiotic therapy, and the use of corticosteroids. A summary of the main antibiotics that are currently recommended in US and UK national guidelines, as well as in large prospective studies, are provided in table 1.
The 2011 Infectious Diseases Society of America national guidelines have now recommended patients with pus forming cellulitis to be treated with antibiotics that target CA-MRSA.
When should a person be admitted to hospital for intravenous antibiotics?
Eron classification v Dundee classification
The Eron classification is based on expert opinions, and is among the most widely used classification systems for diagnosis and treatment of cellulitis.
Table 3 Eron clinical classification system
However, new criteria such as the 2011 Dundee classification are also available. Seventy per cent of people that, based on Eron recommendations, would be treated with inpatient stay and intravenous antibiotics meet the criteria for outpatient management based on the Dundee criteria. Further validation of the Dundee criteria is required.
Outpatient parenteral antibiotic therapy (OPAT)
A prospective study on 344 episodes of treatment administered by a UK OPAT service showed that 87% of patients were cured, readmission rate was 6.3%, and patient satisfaction was high. OPAT costs 41% of inpatient costs when calculated using conservative cost measurements. The authors of the study concluded that clinicians should use OPAT where available; this is supported by CREST guidelines.
When should a switch to oral antibiotics be made?
CREST guidelines suggest indications for a switch to oral therapy are apyrexia (<37.8°C) for 48 hours, regression of cellulitis from a clearly marked area (on daily review), and a falling C reactive protein level.
[Link to free BMJ article PDF for full text, tables, and references]
© 2012 BMJ Publishing Group Ltd





 留言列表
留言列表
 線上藥物查詢
線上藥物查詢 