Purpose: Drug therapies for patients with acute heart failure syndromes (AHFS) are reviewed, including clinical practice guideline recommendations for the treatment of hospitalized patients with heart failure (HF).
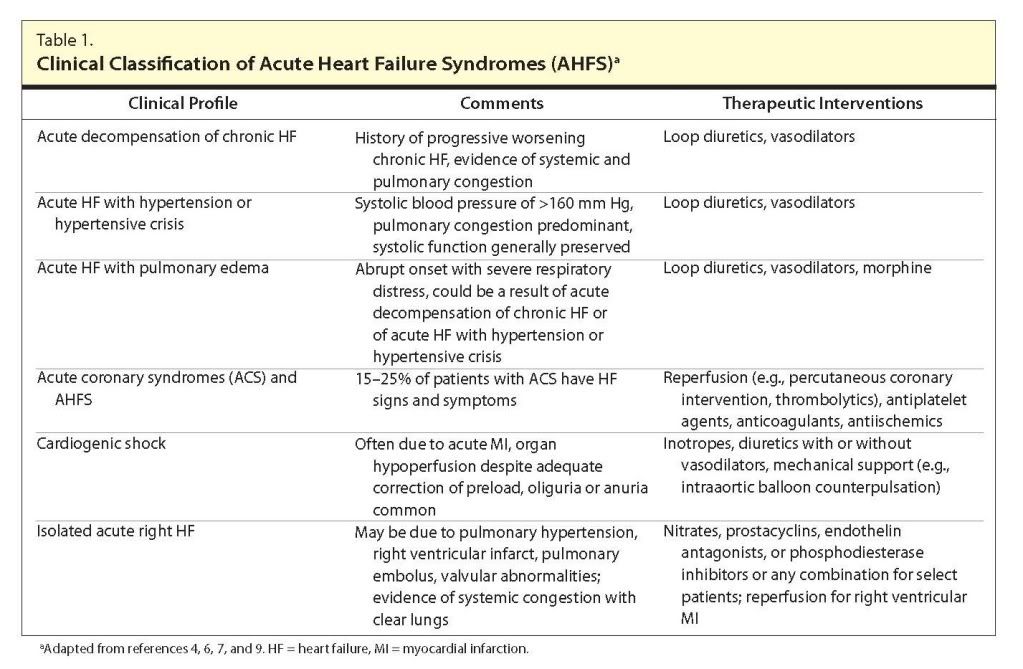
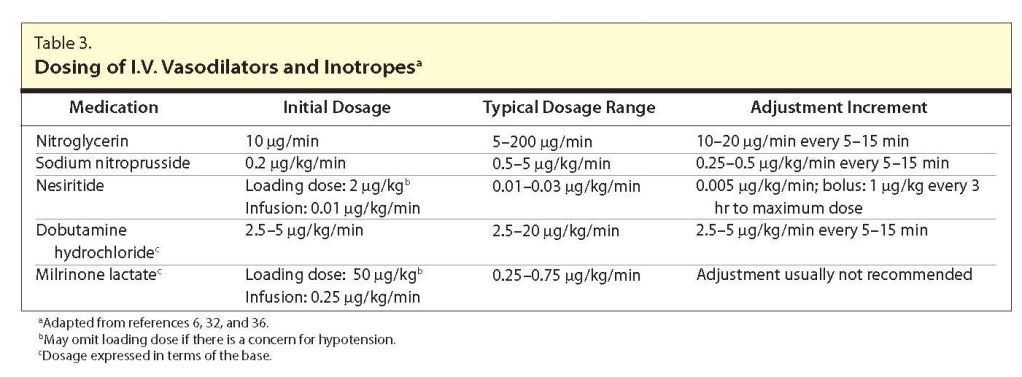
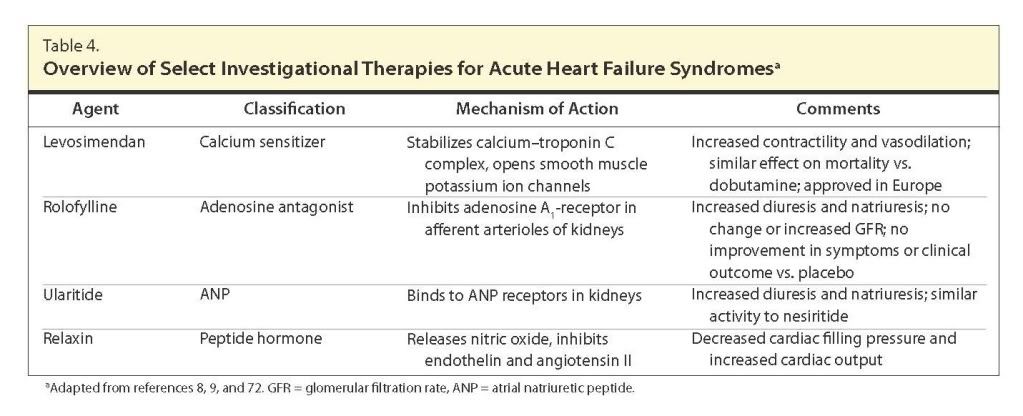
Summary: AHFS may be defined as new-onset, gradual, or rapidly worsening HF signs and symptoms that require urgent therapy. Clinical practice guidelines from the American College of Cardiology Foundation-American Heart Association, Heart Failure Society of America, and European Society of Cardiology offer recommendations for the management of AHFS, addressing the role of diuretics, vasodilators, and inotropes. The guidelines emphasize the utility of vasodilators for patients with signs and symptoms of pulmonary congestion, including pulmonary edema or severe hypertension or both, who have not responded to diuretics. The early initiation of vasoactive medications, including diuretics and vasodilators, has been linked to improved outcomes in some reports. Conversely, the use of inotropes is de-emphasized, particularly as part of the routine management of these patients. Newer agents, including vasopressin antagonists, have also been approved recently but are not addressed by the clinical practice guidelines. The guidelines address the importance of initiating and optimizing evidence-based oral medications for long-term use, including angiotensin-converting-enzyme (ACE) inhibitors, angiotensin-receptor blockers, β-blockers, and aldosterone antagonists, during the patient's hospital stay in an effort to address long-term outcomes.
Conclusion: Drug therapy of AHFS may include diuretics, vasodilators, morphine, ACE inhibitors, digoxin, inotropes, and vasopressin antagonists. Clinical practice guidelines for patients with AHFS provide a useful mechanism to incorporate available evidence and standards of practice into patient care.






 留言列表
留言列表
 線上藥物查詢
線上藥物查詢 