The Facts About Chronic Kidney Disease (CKD)
- 26 million Americans have CKD and another 20 million more are at increased risk.
- Early detection can help prevent the progression of kidney disease to kidney failure.
- Heart disease is the major cause of death for all people with CKD.
- Glomerular filtration rate (GFR) is the best estimate of kidney function.
- Hypertension causes CKD and CKD causes hypertension.
- Persistent proteinuria means CKD.
- High risk groups include those with diabetes, hypertension and family history of kidney disease.
- African Americans, Hispanics, Pacific Islanders, Native Americans and Seniors are at increased risk.
- Three simple tests can detect CKD: blood pressure, urine albumin and serum creatinine.

| Stage | Description | Glomerular Filtration Rate GFR) |
|---|---|---|
| At increased risk | Risk factors for kidney disease (e.g., diabetes, high blood pressure, family history, older age, ethnic group) | More than 90 |
| 1 | Kidney damage (protein in the urine) and normal GFR | More than 90 |
| 2 | Kidney damage and mild decrease in GFR | 60 to 89 |
| 3 | Moderate decrease in GFR | 30 to 59 |
| 4 | Severe decrease in GFR | 15 to 29 |
| 5 | Kidney failure (dialysis or kidney transplant needed) | Less than 15 |
Glomerular filtration rate
Glomerular filtration rate (GFR) is the volume of fluid filtered from the renal (kidney) glomerular capillaries into the Bowman's capsule per unit time.[1]
Glomerular filtration rate (GFR) can be calculated by measuring any chemical that has a steady level in the blood, and is freely filtered but neither reabsorbed nor secreted by the kidneys. The rate therefore measured is the quantity of the substance in the urine that originated from a calculable volume of blood. The GFR is typically recorded in units of volume per time, e.g. milliliters per minute ml/min. Compare to filtration fraction.

There are several different techniques used to calculate or estimate the glomerular filtration rate (GFR or eGFR).
Creatinine clearance approximation of GFR
In clinical practice, however, creatinine clearance is used to measure GFR. Creatinine is produced naturally by the body (creatinine is a metabolite of creatine, which is found in muscle). It is freely filtered by the glomerulus, but also actively secreted by the renal tubules in very small amounts such that creatinine clearance overestimates actual GFR by 10-20%. This margin of error is acceptable considering the ease with which creatinine clearance is measured. Unlike precise GFR measurements involving constant infusions of inulin, creatinine is already at a steady-state concentration in the blood and so measuring creatinine clearance is much less cumbersome.
Calculation of Ccr
Creatinine clearance (CCr) can be calculated if values for creatinine's urine concentration (UCr), urine flow rate (V), and creatinine's plasma concentration (PCr) are known. Since the product of urine concentration and urine flow rate yields creatinine's excretion rate, creatinine clearance is also said to be its excretion rate (UCr×V) divided by its plasma concentration. This is commonly represented mathematically as
Example: A person has a plasma creatinine concentration of 0.01 mg/ml and in 1 hour produces 60ml of urine with a creatinine concentration of 1.25 mg/ml.
Commonly a 24 hour urine collection is undertaken, from empty-bladder one morning to the contents of the bladder the following morning, with a comparative blood test then taken. The urinary flow rate is still calculated per minute, hence
To allow comparison of results between people of different sizes, the CCr is often corrected for the body surface area (BSA) and expressed compared to the average sized man as ml/min/1.73 m2. While most adults have a BSA that approaches 1.7 (1.6-1.9), extremely obese or slim patients should have their CCr corrected for their actual BSA.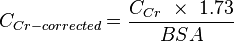
BSA can be calculated on the basis of weight and height
Estimated values
A number of formulae have been devised to estimate GFR or Ccr values on the basis of serum creatinine levels
Estimated creatinine clearance rate (eCcr) using Cockcroft-Gault formula
資料來源:
1.www.kidney.org/kidneydisease/ckd/knowGFR.cfm
2.en.wikipedia.org/wiki/Renal_function#Estimated_values
A commonly used surrogate marker for actual creatinine clearance is the Cockcroft-Gault formula, which may be used to calculate an Estimated Creatinine Clearance, which in turn estimates GFR:[2] It is named after the scientists who first published the formula, and it employs creatinine measurements and a patient's weight to predict the Creatinine clearance.[3][4] The formula, as originally published, is:
For creatinine in µmol/L:
Where Constant is 1.23 for men and 1.04 for women.
Estimated GFR (eGFR) using Modification of Diet in Renal Disease (MDRD) formula
The most recently advocated formula for calculating the GFR is the one that was developed by the Modification of Diet in Renal Disease Study Group.[5] Most laboratories in Australia,[6] and The United Kingdom now calculate and report the MDRD estimated GFR along with creatinine measurements and this forms the basis of Chronic kidney disease#Staging.[7] The adoption of the automatic reporting of MDRD-eGFR has been widely criticised.[8][9][10]
The most commonly used formula is the "4-variable MDRD" which estimates GFR using four variables: serum creatinine, age, race, and gender.[11] The original MDRD used six variables with the additional variables being the blood urea nitrogen and albumin levels.[5] The equations have been validated in patients with chronic kidney disease; however both versions underestimate the GFR in healthy patients with GFRs over 60 mL/min.[12][13] The equations have not been validated in acute renal failure.
For creatinine in mg/dL:
For creatinine in µmol/L
A more elaborate version of the MDRD equation also includes serum albumin and blood urea nitrogen (BUN) levels: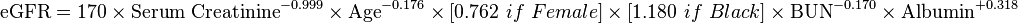
Estimated GFR for Children using Schwartz formula
In children, the Schwartz formula is used.[14][15] This employs the serum creatinine, the child's height and a constant to estimate the glomerular filtration rate:
The method of selection of the K-constant value has been questioned as being dependant upon the gold-standard of renal function used (i.e. creatinine clearance, inulin clearance etc) and also may be dependant upon the urinary flow rate at the time of measurement





 留言列表
留言列表
 線上藥物查詢
線上藥物查詢 